Retro-Odontoid Pseudotumor Formation in the Context of Various Acquired and Congenital Pathologies of the Craniovertebral Junction and Surgical Techniques
Article information
Abstract
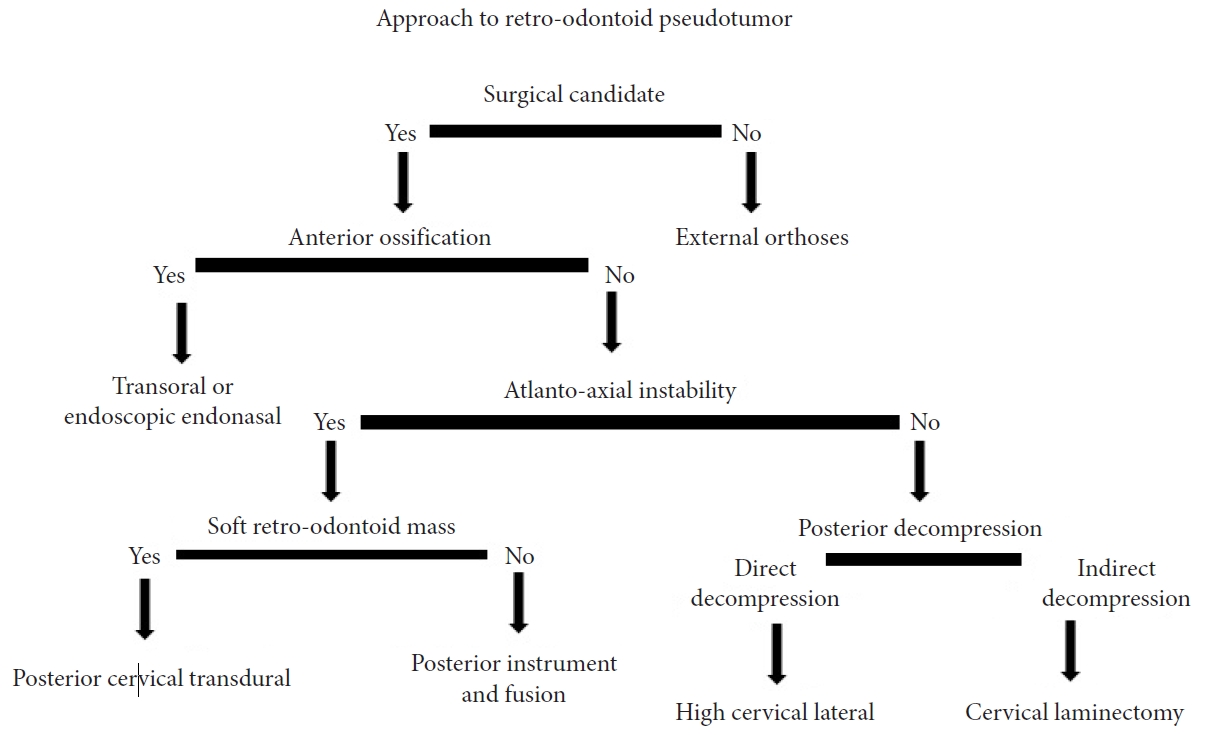
Retro-odontoid pseudotumor formation consists of an abnormal growth of granulation tissue typically posterior to the odontoid process, resulting as a manifestation of atlantoaxial instability. This instability can occur as a result of conditions ranging from severe mechanical trauma to metabolic disease or autoimmune conditions such as rheumatoid arthritis. A pseudotumor may impinge on the spinal nerves or even the spinal cord and brainstem, manifesting symptoms from severe neck pain to cervicomedullary compression or myelopathy, and in some cases even sudden death. The objective of this review is to consolidate the findings in published case reports and relevant prior literature reviews regarding the formation of retro-odontoid pseudotumor. We address the pathophysiology involved in acquired and congenital pseudotumor formation, including those associated with rheumatoid arthritis (panni). Additionally, we discuss past and current operative techniques designed to curtail and ultimately regress a retro-odontoid pseudotumor and pannus. Surgical techniques that are addressed include ventral decompression (both transoral and transnasal), dorsal decompression, and indications for posterior instrumentation in pannus formation, particularly in cases that may be sufficiently treated in lieu of an anterior approach. Finally, we will examine the role of external orthoses as both a method of conservative treatment as well as a potential adjunct to the aforementioned surgical procedures.
INTRODUCTION
Retro-odontoid pseudotumor, or odontoid pannus, refers to a disease process characterized by non-neoplastic soft tissue proliferation that is adjacent to the odontoid process of cervical 2 (C2) vertebra, and can lead to compression of the vital neuronal structures of the cervicomedullary region [1,2]. Anderson and D’Alonzo first classified odontoid fractures associated with pannus formation into 3 types in 1974 [3]. Following its initial discovery, suggested treatment was through a transoral approach for direct removal and decompression of the pannus. However, there existed a significant risk for complications, including cerebrospinal fluid (CSF) leakage and postoperative infections [4]. Surgeons have been shifting towards minimally invasive approaches, including use of endoscopy and upper cervical spinal fusion and laminectomy for indirect decompression [4].
Pseudotumor formation can be secondary to a variety of etiologies. The most common causes include rheumatoid arthritis (RA), acute trauma, and congenital abnormalities such as Down syndrome, Morquoi Syndrome, and neurofibromatosis. In the setting of RA, inflammatory infiltrate of synovial joints leads to buckling of the posterior longitudinal ligament (PLL), causing pannus formation [5]. In cases of acute neck trauma and congenital abnormalities, development of atlantoaxial instability (AAI) causes facet misalignment. This misalignment leads to a reduction in the joint space lateral to the facets which result in a buckling of the PLL, thus propagating an accumulation of retro-odontoid tissue and potential progression to pannus [5]. A pannus can extend into the spinal canal, causing compression of the brainstem and spinal cord leading to myelopathy. This can manifest as weakness, incomplete paresis, and quadriplegia. In severe cases, sudden death may result from vascular insufficiency and brainstem compression [6].
Correct diagnosis of a retro-odontoid pseudotumor or pannus is crucial to avoiding further disease progression. If left untreated, growing pseudotumor/pannus can induce further spinal cord compression, exacerbating neurological symptoms. Early recognition of cervical myelopathy along with swift surgical evaluation can lower morbidity and improve symptomatic outcomes [6]. Evaluating the progression of this disease process, its clinical significance, and surgical treatment approaches will be the focus of this review.
PATHOPHYSIOLOGY
Soft tissue proliferation in the region of the transverse ligament of the atlantoaxial (AA) junction, or pseudotumor, is associated with a diverse list of congenital and acquired conditions (Fig. 1). Historically, pseudotumor has been classified as either rheumatoid or nonrheumatoid in etiology. When associated with RA, pseudotumor may be referred to as pannus. An examination of the histopathology of retro-odontoid pseudotumors associated with 11 different underlying etiologies found great diversity in their composition, suggesting that there may be variability in the underlying processes leading to the proliferation of soft tissue in each condition [1]. However, many of these underlying etiologies result in chronic and/or repetitive injury to the AA joint and associated ligaments; it is the longstanding attempt by the body to repair damage that causes pseudotumor, with histopathology commonly demonstrating pseudotumor composed of a combination of cells associated with the underlying condition as well as inflammatory cells, fibrous cells, and granulation tissue [1,7].
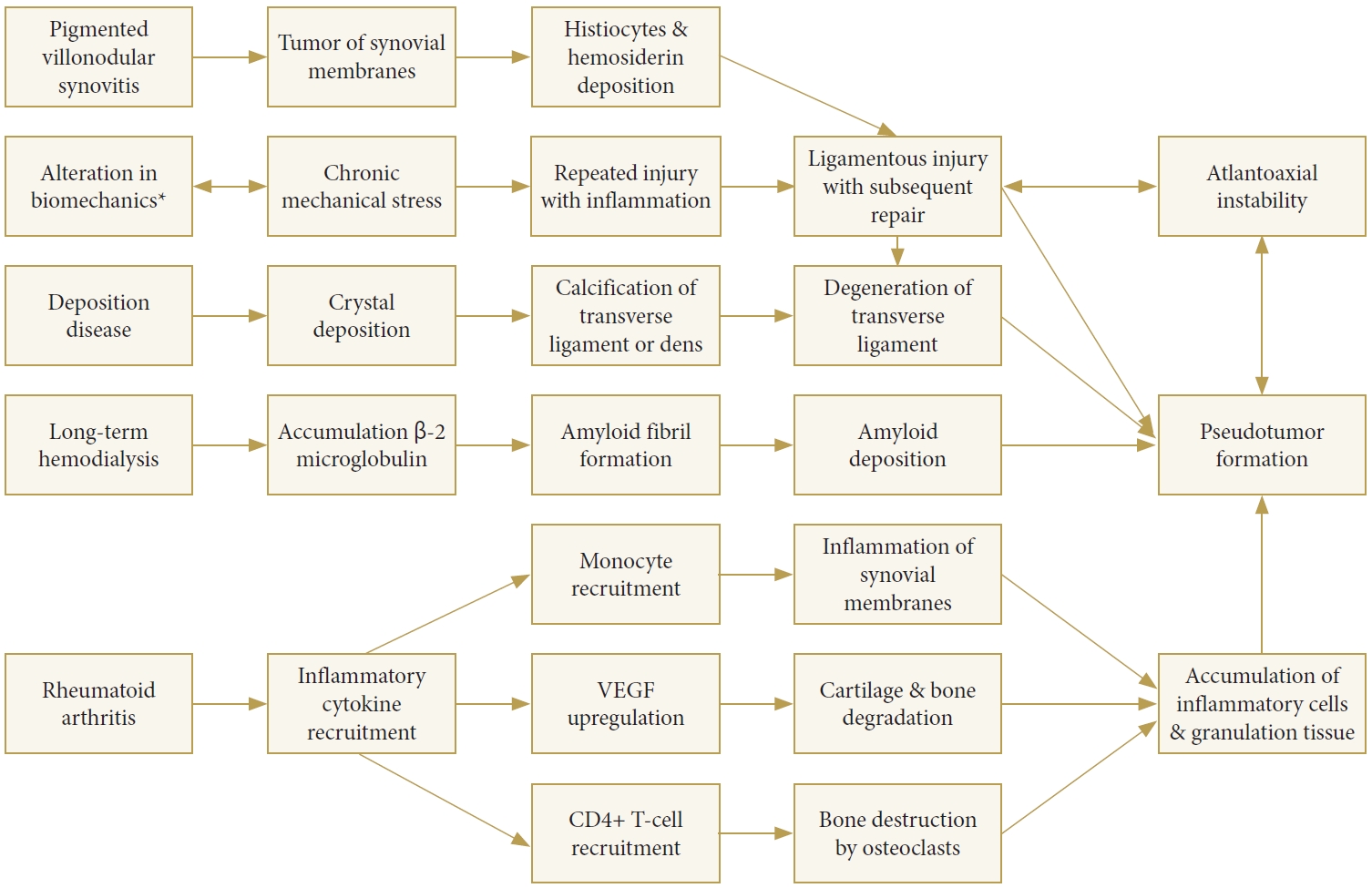
Pathogenesis of retro-odontoid pseudotumor as a result of rheumatoid and nonrheumatoid etiologies. VEGF, vascular endothelial growth factor. *Includes chronic mechanical stress as induced by acute trauma, diffuse idiopathic skeletal hyperostosis, ossification of the posterior longitudinal ligament, and cervical spondylosis.
Three subtypes of RA-associated pannus are known, classified based upon histopathology as hypervascular, hypovascular and fibrous pannus, also known as inflammatory, combined, and fibrous pannus, respectively [1]. RA results in the production of pro-inflammatory cytokines. As a result, synovial membranes are damaged by monocytes, while bone is destroyed by osteoclasts activated by CD4+ T cells [7,8]. Angiogenesis prompted by inflammatory cytokine vascular endothelial growth factor has been found to play a critical role in initiation and propagation of pannus due to its role in vascular permeability as well as cartilage and bone degradation, contributing to the aforementioned cycle of damage and repair [1,7,9].
Retro-odontoid pseudotumor is also associated with AAI of various causes, and trauma. As with instability, any alteration in biomechanics of the cervical spine may result in pseudotumor formation by way of repeated injury with inflammation, resulting ligamentous injury and subsequent repair. Pseudotumor-associated with diffuse idiopathic skeletal hyperostosis (DISH), ossification of the posterior longitudinal ligament (OPLL), and cervical spondylosis are thought to occur by the same mechanism. DISH and OPLL result in a decreased range of motion (ROM) of the subaxial cervical spine with resulting compensatory hypermobility of the craniocervical junction. Trauma may result in nonunion and pseudoarthrosis of an odontoid fracture [10] The most common type of odontoid fracture associated with nonunion or malunion is type II, which occurs at the junction of the axis body and odontoid base [11]. Increased motion at the fractured portion as well as malalignment predisposes to chronic irritation, resulting in fibrous soft tissue mass surrounding the fracture site. In 2007, Sinha et al. [3] compiled 22 studies of retro-odontoid pseudotumor following odontoid fractures, and showed that these masses regressed spontaneously after surgical fixation. This alteration in biomechanics of the occipitoatlantal and AA joint leads to repetitive injury to the joint(s) and associated ligaments and thus, retro-odontoid pseudotumor formation.
In addition, deposition diseases, such as calcium pyrophosphate dihydrate deposition disease (CPPD), gout, and amyloid arthropathy may cause pseudotumor. The underlying disease process of CPPD, referred to as chondrocalcinosis, involves the deposition of calcium pyrophosphate dihydrate crystals in ligaments, synovium, and capsule structures [12]. In the cervical spine, these crystals may deposit into the transverse ligament, longitudinal ligament, intervertebral discs, facet joints, and annulus fibrosis, manifesting as linear diffusely distributed calcifications. One severe manifestation of CPPD is calcifications surrounding the apex of the dens, termed “crowned dens syndrome,” presenting clinically with occipital pain and neck stiffness [13]. On magnetic resonance imaging (MRI), it can be difficult to distinguish chondrocalcinosis from other causes of retro-odontoid pseudotumor, and on histological analysis, these masses are composed of inflammatory cells with positive birefringent rhomboid shaped crystals [14].
Additionally, hemodialysis-associated amyloidosis may cause pseudotumor. For patients on long-term dialysis, accumulation of β-2 microglobulin in the form of amyloid fibrils in joints and surrounding structures can occur. These fibrils can accumulate in the cervical spine, and deposit in the craniocervical junction [15]. The inflammatory deposits and amyloid can subsequently lead to development of retro-odontoid pseudotumor [16]. Lastly, there have been prior case reports of pigmented villonodular synovitis (PVNS) as a cause of retro-odontoid pseudotumor [17]. PVNS is a proliferative, destructive, nonmalignant tumor of synovial membranes that can affect the cervical spine in up to 36% of cases [18]. Histopathologically, these lesions are noted to have mononuclear histiocytes intermixed with multinucleated giant cells and hemosiderin deposition [19,20]. The resulting inflammation and joint degeneration again drive pseudotumor initiation and propagation.
IMPORTANT STRUCTURAL AND FUNCTIONAL CONCERNS FOR STABILITY
Retro-odontoid pseudotumor formation results in structural and functional concerns that coincide with AAI, which can be assessed clinically and radiographically. AA subluxation, one of the most common causes of pseudotumor formation, can manifest as minor axial neck pain with progressive sequelae occurring as the degree of instability worsens, and eventually may result in death [21]. Neck pain, limitations in ROM, numbness/weakness, and pyramidal signs are some of the more common symptoms of instability. Additional symptoms of pseudotumor-associated instability include sphincter disturbances, respiratory distress, and lower cranial nerve dysfunction [21]. A thorough physical exam and workup of the underlying etiology of pseu-dotumor formation are important.
AAI associated with retro-odontoid pseudotumor formation displays radiographic features that allow the physician to improve preparedness for intervention and patient outcomes. Acquisition of dynamic conventional radiographs in flexion, neutral, and extension are used for the evaluation of the atlantodental interval (ADI), which is defined as the distance between the anterior tubercle of C1 and the anterior aspect of the odontoid process [21]. In addition, these radiographs can be used to analyze ROM, as well as for evaluation of basilar invagination by way of the McGregor line, a line passing through the anterior and posterior arches of the atlas, and the line parallel to the endplate of the vertebrae [22]. Although there is no definite criterion, a retrospective analysis performed by Yamada et al. [23] in 2019 used the criterion of an ADI of 5 mm or more for AA subluxation.
MRI can be used to visualize the pseudotumor, typically ranging from isointense to hypointense relative to the spinal cord on T1-weighted images and hypointense in T2-weighted images [22]. T2-weighted images can also be used to evaluate deterioration of the transverse ligament, suggesting the pathogenesis is taking place [24]. Computed tomography (CT) and CT angiograms are commonly acquired preoperatively, with one study performed by Barbagallo et al. [25] showing an eggshell calcification of the pseudotumor. Postoperative imaging is acquired to ensure proper placement of instrumentation, pseudotumor removal, and decompression of the spinal cord, when applicable. In the follow-up period of the study by Barbagallo et al. [25], serial MRIs were obtained to track pseudotumor size reduction and further improvement of spinal cord compression at 4, 10, and 14 months. Likewise, in clinical practice, a thorough and consistent radiographic regimen from initial presentation through follow-up period is necessary to monitor the patient’s condition and ensure desired results.
OPERATIVE TECHNIQUES
1. Ventral Decompression
There are a variety of pathologies resulting in the compression of the anterior upper cervical spinal cord. The most common condition necessitating surgical intervention for ventral cord compression is development of an inflammatory pseudotumor [26]. Improvements in biologic agents for the treatment of RA have decreased the incidence of pannus formation [26-29]. However, pseudotumor formation often has an insidious onset, allowing for the formation of lesions leading to neurological compromise and potential craniovertebral junction (CVJ) instability. While in some cases pseudotumor regression can be achieved by upper cervical spine stabilization alone, ventral decompression via a transoral (TO) or endoscopic endonasal (EE) approach is indicated in cases of severe anterior decompression that cannot be addressed by a posterior-only procedure [26,30-33]. Likewise, ventral decompression is necessary in patients with calcification ventral to the odontoid process (Fig. 2) [26,32]. In these cases, stabilization without direct decompression does not lead to improved neurologic outcomes.
Cervical pseudotumor formation most often occurs adjacent to the dens. Common locations include between the anterior arch of C1 and the dens, and between the transverse ligament and the dens [26,30,34]. Surgical access to retro-odontoid pseudotumor is achieved by varying degrees of resection of the odontoid process and/or anterior arch of C1. Reported combinations include partial odontoidectomy with or without preservation of C1, odontoidectomy with or without C1 arch preservation, and rarely, sparing of the dens. Partial drilling at the inferior portion of the anterior arch of C1 has also been reported [27,31].
Historically, the transoral approach to the CVJ has been the gold standard to achieve anterior decompression in this region [35-37]. A transoral procedure results in a plane with a slight anterior-posterior skew off of a craniocaudal approach relative to the odontoid process; this is what typically necessitates resection of the anterior arch of C1. Conversely, an EE approach permits a purely craniocaudal approach to the dens, thereby preserving C1 and in some cases, the dens itself, even when the pathology being treated is in a retro-odontoid location [35].
Partial odontoidectomy with preservation of the anterior arch of C1 aims to limit if not elude iatrogenic instability, sometimes allowing avoidance of posterior fixation and its associated risks. Notably, disruption of bony mechanics as well as soft tissue articulations may lead to clinically significant instability [35,38]. The alteration in biomechanics of the AA axis following resection of the odontoid and associated ligaments such as the transverse and alar ligaments as well as the tectorial membrane unsurprisingly results in significant increases in degrees of flexion, extension, and lateral bending [35]. An in vitro study by Dickman et al. [39] demonstrated as a result of the change in the degrees of rotation at C1/C2, odontoidectomy resulted in a redistribution of the axes in which rotation occurred. Following odontoidectomy, rotation at C1/C2 was redistributed across the entire body of C2, a profound derangement of the naturally occurring biomechanics. Partial resection of the odontoid and C1 is far less common, but an illustrative case is presented in Fig. 3.
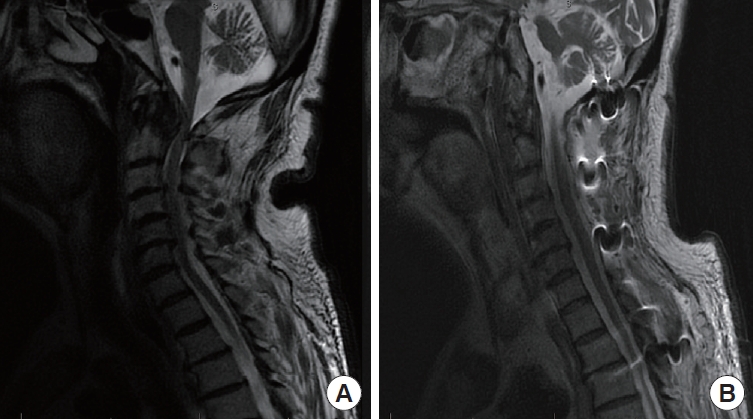
Illustrative case of a patient with past medical history of rheumatoid arthritis presenting with severe posterior neck pain and bilateral hand weakness. (A) Preoperative midsagittal T2-weighted magnetic resonance imaging (MRI) shows retro-odontoid pannus with compressive upper cervical spinal cord stenosis, along with subaxial cervical stenosis. (B) Postoperative midsagittal T2-weighted MRI shows resultant transnasal resection of pannus. Additional C1–6 decompressive laminectomy and occipital-T2 instrumentation and fusion were performed due to subaxial cervical stenosis.
Duntze et al. [36] reported 3 cases of EE partial odontoidectomy in which they allowed the C1 anterior arch to remain intact, thereby limiting occipito-atlantal instability for treatment of rheumatoid pannus. Fixation was avoided in all 3 patients due to surgical concerns of patient frailty. These patients presented with no pre- or postoperative instability, were able to comply with regular radiological follow-up, and had pseudotumor formation located posterior to the dens. While all 3 patients demonstrated rapid neurological improvement postoperatively with no evidence of cervical instability, the authors note that C1/C2 fusion remains their preferred practice with exceptions made only for the aforementioned rare indications. Gladi et al. [31] reported EE odontoidectomy (EEO) and rheumatoid pannus removal in an elderly patient with C1 anterior ring preservation resulting in neurological improvement, no evidence of cervical instability, and no posterior fusion at 1-year follow-up. The group would later publish a follow-up case series of 7 patients who received EEO with preservation of C1 for rheumatoid pannus and associated basilar invagination. All 7 patients forewent posterior fixation, while 2 patients received anterior fusion. With a minimum of 4.5 years and an average of 66.2 months of follow-up, none of the patients demonstrated radiological or clinical signs of CVJ instability [40]. Joaquim et al. [26] reported their practice preference often allows for preservation of the superior 25% of the anterior arch of C1, although case numbers were not provided. Abdelgawaad et al. reported 2 cases in which they accessed the retro-odontoid space for epidural abscess drainage and debridement without completing odontoidectomies [35]. This was achieved through a combined endoscopic transnasal and transoral approach which allowed the surgeons to access the pathology by way of a plane created through the soft tissue between the odontoid process and the clivus. The superior crus of the cruciform ligament was resected, while all other ligaments, including those most crucial to the stabilization of the CVJ were spared. A 2015 systematic review by Platt et al. [38] which included the former 2 cited studies reported 17 cases in the literature of endoscopic endonasal approach (EEA) with C1 arch preservation, 9 of which did not require fixation.
Nevertheless, Edwards [41] reported a case of fatal atlantoaxial instability following an odontoid sparing TO decompression. Barring major contraindications that would necessitate a single-stage anterior decompression, it remains the standard to couple fixation with decompression.
The range of access provided by TO and EE approaches differs significantly. The nasopalatine line (NPL) is the inferior boundary for EE procedures. While the NPL may vary with respect to spinal level from patient to patient, the TO approach provides greater caudal access than EE surgery. The TO approach is limited relative to EEA superiorly; this boundary may be extended by splitting the hard and soft palate. However, this may result in velopharyngeal insufficiency (VPI) [38,42-44]. Analogous extension of the range of instruments in EEA is achieved by resection of the middle and inferior nasal turbinates and nasal septum [37,38]. Associated complications include nasal crusting and increased rates of upper respiratory infection [38].
In addition to a plane more favorable for C1 arch preservation, the EEA has the added benefit of mucosal incisions in the nasopharynx (versus TO which incises the oropharynx) [35,38]. A decreased likelihood of trauma to retropharyngeal tissues in EEA and improved oropharyngeal function postoperatively has been demonstrated to result in less overall time intubated, faster return to feeding, decreased overall recovery time, and shorter length of stay (LOS) [35,38,44]. Avoidance of excessive retraction of the posterior pharyngeal wall and tongue may minimize tissue trauma and postoperative swelling [31,38,42,45-48]. Standard use of an endoscope in the endonasal approach thereby providing better visualization of the surgical field has been cited in favor of EEA in comparison to TOA, which may use endoscopy but more commonly uses a microscope, which may have the field of view partially obstructed by the hard palate [35,38].
Both approaches are limited by a steep learning curve and potential for severe neurological morbidity and mortality, with a particularly intimate relationship between the surgical corridor and the brainstem in an EEA. A 2016 meta-analysis and systematic review found that tracheostomy was the most common surgically-related complication associated with transoral odontoidectomy (TOO), occurring in 10.8% of patients [43]. One of the included studies by Marda et al. noted that preoperative lower cranial nerve palsies and respiratory symptoms as well as longer surgery times and intraoperative blood transfusions contributed to a greater likelihood of pulmonary complications in TOO [22,49]. Other TOA complications (excluding hardware-related issues) included dysphagia, VPI, wound dehiscence, arterial injury, meningitis, and CSF leak. By comparison, EEA complications listed in most common to least commonly occurring included CSF leak, gastrostomy, meningitis, dysphagia, VPI, and tracheostomy [35,43,44]. Thirty-day mortality rates for TOO and EEA were 2.9% and 4.4%, respectively. Challenges associated with EEA are limitations to access and intraoperative field of view for management of intraoperative complications. Specifically, lack of hemostasis or vascular injury (which is extremely rare in this approach) can quickly obscure the endoscope, and endoscopy remains at a disadvantage for time-sensitive changes in instrumentation. Lack of ability to achieve primary closure of the dura via suturing necessitates use of fat grafts and fibrin glue, with potential for CSF fistula formation [38]. Postoperative use of a lumbar drain has been cited in the literature as further means of management of CSF leak incurred during both types of procedures, though many note they do not routinely do so [26,42,45,46,50,51]. Rates of VPI may be underreported in both approaches given that the pathophysiology includes iatrogenic fibrosis of the soft palate and pharyngeal wall, which may not present clinically until three to 6 months postoperatively [43]. In this study, underlying pathologies prompting surgical intervention were not limited to rheumatoid pannus.
2. Dorsal Decompression
AAI may both contribute to and result from pseudotumor formation. In cases with AAI, posterior fixation to address the instability is indicated. Reports of pseudotumor regression following surgical fixation alone without direct resection of the lesion are widespread in the literature; techniques for posterior instrumentation as treatment of pseudotumor are discussed below.
There are many etiologies causing symptomatic retro-odontoid pseudotumor without inherent instability of the CVJ or cervical spine. In these instances, posterior approach options include reduction of the lesion via posterior decompression without fixation or direct resection of the lesion. The former has been demonstrated with both C1 laminoplasty or laminectomy without use of any instrumentation or fusion [52,53]. In these case series, indication for decompression of C1 included instances when instrumentation was unfavorable as in the case of high riding vertebral artery and preserving ROM in patients without AAI [52,53]. Suetsuna et al. [52] published a small case series of 3 patients who underwent C1 laminoplasty. All patients demonstrated improvement in their Japanese Orthopedic Association (JOA) scores for cervical myelopathy. Furthermore, one patient showed radiographic reduction of pseudotumor with complete resolution of pseudotumor in the other 2 patients. Patients were followed-up for 25–33 months and no postoperative complications, including progressive cervical kyphosis or recurrence or enlargement of pseudotumor, were reported [52]. Kakutani et al. [53] published a case series of 7 patients who underwent C1 laminectomy without instrumentation and fusion. In all patients, there was an improvement in the in the JOA scores. Four of the 5 patients who received MRI during a postoperative workup confirmed complete reduction of pseudotumor within 1 year without recurrence. In this series, patients were followed for up to 4 years and surgery demonstrated mild kyphotic changes at the occipital-cervical (O-C) junction and in the subaxial cervical spine, however, none of these patients required correction of kyphotic deformity.
Another option for cases not requiring fusion is the high cervical lateral approach as first described by Henry in 1973 for C1–2 vertebral artery access. Naito et al. [54] described 3 cases in which nonrheumatoid retro-odontoid pannus were partially resected via this approach. All 3 patients demonstrated improvement in symptoms and no recurrence after a minimum of 3 months and maximum of 2 years of postoperative scans. Limitations to this approach include inability to achieve complete resection in instances where that may be necessary, recommendation to extend no further caudally than the C3 level, a deep, narrow field of view, risk to the vertebral artery, facial and accessory nerve as well as their associated branches, and necessary resection of the C2 nerve root when it crosses the operative field. However, for lesions large enough to cause significant mass effect requiring decompression by direct resection, the posterolateral approach may remain a useful option. Oohori et al. [55] discussed a case in which a 67-year-old patient with rheumatoid pannus underwent a left unilateral laminectomy from C1–3; they were unable to visualize the mass due to mass effect on the cord obstructing their approach. Subsequently, they repositioned the patient and were able to remove the mass via posterolateral approach via resection of part of the left occipital bone and partial resection of the posterior aspect of the C1–2 facet joint. The patient’s symptoms improved and follow-up imaging demonstrated cord decompression with no C1–2 instability at 12-month postoperation.
A posterior transdural approach for resection of a ventrally located lesion was described in the literature as early as 1910 by Taylor [56] for resection of an intradural lesion by way of a unilateral hemilaminectomy. Since that time, a posterior transdural approach has been utilized for a variety of extradural ventral lesions, including herniated discs, cysts, and retro-odontoid pseudotumor [57]. Consideration of this approach for treatment of pseudotumor requires evaluation of factors unique to this pathology. Calcification of the lesion as demonstrated on CT and imaging suggesting adherence of the lesion to dura and/or surrounding tissue are contraindications to a posterior transdural approach posing an increased risk of CSF leak and damage to surrounding tissue. Soft, mucoid, or fibrous lesions are well suited for transdural resection. Likewise, though a posterior transdural approach has been utilized in patients with and without instrumentation, that the approach requires a posterior midline incision is conducive to accommodating addition or extension of fusion and instrumentation when necessary. A transdural approach also has the benefit of not requiring retraction on the spinal cord itself. Other considerations for this approach include the requirement of intraoperative ultrasound and neuromonitoring as well as a steep learning curve necessitated by that of a microsurgically trained spinal surgeon with intradural resective experience.
POSTERIOR INSTRUMENTATION FOR TREATMENT OF PSEUDOTUMOR FORMATION
1. Occipital-Cervical Fusion
The techniques utilized for treating pseudotumor formations using posterior instrumentation includes O-C fusion as well as C1–2 fusion. The goal with posterior instrumentation is to achieve a similar level of success in pseudotumor regression compared anterior and circumferential approaches, along with comparable clinical improvements in Nurick scoring, while minimizing postoperative complications and recovery times [58]. O-C fusion is indicated in cases where panni impinge on the medulla and upper cervical cord as a result of cranial settling, leading to subaxial subluxation or extensive destruction of the atlanto-occipital joint [59,60]. Patients typically present with cases of severe neck pain and myelopathy secondary to the aforementioned subluxation, which can progress to sudden death [61,62]. MRI may also indicate erosion of the odontoid process, further indicating surgical intervention with posterior instrumentation due to implied C1–2 instability [61]. Additionally, concomitant CVJ instability or destruction of the atlanto-occipital joint regularly warrants O-C fusion as transnasal approaches for decompression without stabilization are found to be inadequate in maintaining long-term stability [63].
The goal in occipital surgical fusion is to prevent further progression of the pseudotumor and improve neurological outcomes; this is achieved by use of intraoperative monitoring as the surgeon slowly decompresses the medulla to prevent tissue damage [12]. Neurological improvements are often noted in patients as soon as 1 week after surgery and complete resolution of the pseudotumor can be visualized on imaging within one year of surgical repair [12]. In a review of Winegar et al. [64], 64.5% of patients reported overall improvement in Ranawat and Frankel grading of neurologic status as well for Denis pain classification. Improvements in patient satisfaction were noted in 85.9% of patients as determined by Conaty and Mongan grading scales. These results, when combined with low rates of instrumentation failure provide an effective treatment option for patients with pseudotumor formation severely affecting the atlanto-occipital joint [59,60].
2. C1–2 Fusion
The C1–2 synovial lining around the odontoid is one of the most common regions for pseudotumor formation [12]. In the case of C1–2 fusion, posterior instrumentation is indicated for cases of AAI as a result of retro-odontoid pseudotumor as documented on MRI [65]. The goal is to stabilize the C1–2 level of the spinal axis to prevent further expansion of, and ultimately regress inflammatory granulation tissue before neurologic symptoms present or progress [32]. Further indication for C1–2 fusion is to curtail progressive degeneration of the transverse ligament resulting in forward slippage of the atlas over the axis that would eventually progress to irreducible atlantoaxial kyphosis [60]. A study of 22 patients requiring C1–2 fusion by Grob et al. [65] found 20 of said patients presented with intractable pain with 9 of those patients also presenting with concurrent myelopathy, only in this case secondary to the aforementioned AAI. C1–2 fusion is an ideal approach when there is no concomitant calcification ventral to the odontoid, for which ventral decompression is more appropriate [32,39]. The main benefit with C1–2 fusion is that this procedure has a more conservative approach than transoral/transpharyngeal resections yet offers the possibility of a satisfactory level of pseudotumor reabsorption, leading to a reduction and in some cases an absence of neurologic symptoms postoperation as determined by the Nurick scoring scale [58,66].
EXTERNAL ORTHOSES
External orthoses have been used independently as a conservative measure and in conjunction with surgery as a routine postoperative treatment. Although there are different types, collars are used to limit motion, to reduce graft loading and migration, and to encourage fusion [67]. External orthoses used conservatively can be utilized to potentially correct, improve, or prevent progression of an existing deformity, to stabilize and immobilize weak or damaged spinal segments, to reduce the axial load of the spine, and to limit unnecessary motion [68]. Although surgical intervention for cervical pseudotumor is typically utilized in most patients, a conservative option using only external orthoses to stabilize the cervical spine can be a viable option for patients who cannot undergo surgery or when surgery is technically challenging [67]. Conservative treatment mandates use of a rigid collar for 8 weeks, followed by use of a soft collar for an additional 4 weeks. It is also recommended that pseudotumor formation should be monitored by cervical CT imaging every month for the first 3 months as well as every 2 months over the course of one year [33].
In a survey of North American spine surgeons, 63% stated they routinely use orthoses after cervical spine operations, the primary purpose of which is to limit cervical spinal motion in order to allow for proper union and healing [69]. The frequent postoperative use of orthoses on the cervical spine allows the surgeon to stabilize the high degree of mobility of the cervical spine (as it pertains to daily movement and activity) and also to reduce the load on the segment involved in cervical fusion in order to increase successful fusion rates [68]. A case study by Oseni et al. [33] also describes external orthoses as a conservative measure to treating pseudotumor formation at C2 in a 73-year-old female with seronegative polyarthritis. Following a surgical decompression and laminectomy, the patient was instructed to use a rigid cervical collar for 8 weeks with the subsequent use of a soft cervical collar for 4 weeks. At the end of postoperative external orthoses use, the pseudotumor had decreased from 11 mm to 5 mm, along with reduction of pain. These findings are supported by additional studies showing substantial regression of pseudotumor in patients who were treated with postoperative external orthoses [70-72].
CONCLUSION
Retro-odontoid pseudotumor is an uncommon entity with a diverse set of underlying etiologies, including inflammatory conditions such as RA, as well as nonrheumatological causes such as odontoid fracture, OPLL, DISH, CPPD, and PVNS. A key feature of retro-odontoid pseudotumor pathogenesis is the repeated cycle of ligamentous injury and repair, thought to be initiated most commonly by damage to the transverse ligament as a result of inflammation, trauma, degeneration, and/or an alteration in biomechanics. Clinical manifestations can be broad depending on the severity and specific etiology of the underlying cause and local disease. Regardless, accurate and timely diagnosis is essential to initiate prompt treatment, with the primary objective being to lower morbidity and improve symptomatic outcomes. Despite this being a rare entity, the most common reason for surgical intervention in the case of spinal cord compression is presence of an inflammatory pseudotumor. Irrespective of etiology, a phenomenon that has been observed is the regression of pannus postoperatively after fusion, indicating that excess motion at the craniocervical junction may be a driving factor in retro-odontoid pseudotumor development and progression.
A retro-odontoid pseudotumor or pannus may be treated via various approaches to access the pannus to achieve either ventral or dorsal decompression (Supplementary Table 1). Alternatively, it may be treated with a single-step fixation procedure alone. Regardless if decompression is performed and independent of the approach taken to do so, posterior fixation is generally considered an essential component of treatment, either as part of a 2-step procedure, or performed in isolation. This is due both to the high potential for iatrogenic instability as introduced by decompression, as well as the role of AAI in pannus progression. Pharmacological advancements in the form of biologics for treatment of RA also show great promise, and there exists a decreased incidence of pannus in the general population. However, there would be great benefit for future studies to further elucidate the pathophysiology of retro-odontoid pseudotumor in order to allow for earlier recognition of this disease, improvement of neurological outcomes, and continued development of minimally invasive surgical treatments.
Notes
The authors have nothing to disclose.
SUPPLEMENTARY MATERIALS
Supplementary Table 1 can be found via https://orcid.org/ns.2040402.201.