 |
 |
- Search
| Neurospine > Volume 18(4); 2021 > Article |
|
|
Abstract
Thoracolumbar spine is the most injured spinal region in blunt trauma. Literature on the indications for nonoperative treatment of thoracolumbar fractures is conflicting. The purpose of this systematic review is to clarify the indications for nonsurgical treatment of thoracolumbar fractures. We conducted a systematic literature search between 2010 to 2020 on PubMed/MEDLINE, and Cochrane Central. Up-to-date literature on the indications for nonoperative treatment of thoracolumbar fractures was reviewed to reach an agreement in a consensus meeting of WFNS (World Federation of Neurosurgical Societies) Spine Committee. The statements were voted and reached a positive or negative consensus using the Delphi method. For all of the questions discussed, the literature search yielded 1,264 studies, from which 54 articles were selected for full-text review. Nine studies (4 trials, and 5 retrospective) evaluating 759 participants with thoracolumbar fractures who underwent nonoperative/surgery were included. Although, compression type and stable burst fractures can be managed conservatively, if there is major vertebral body damage, kyphotic angulation, neurological deficit, spinal canal compromise, surgery may be indicated. AO type B, C fractures are preferably treated surgically. Future research is necessary to tackle the relative paucity of evidence pertaining to patients with thoracolumbar fractures.
Thoracolumbar spine fractures occur in every 7/10 blunt trauma cases and make up to 9/10 of the spinal fractures recorded [1-5]. Every 1 in 4 thoracolumbar spine fracture patients have concomitant spinal cord injury [1,4]. Long-term care in cases with persistent disability post thoracolumbar fractures indicates a significant burden on healthcare funding [1,2,4-6]. Furthermore, such cases often have numerous visceral and bony injuries, and therapeutic decision-making can be quite demanding [4,6].
For the aims of these recommendations, “thoracolumbar” includes the rigid thoracic (T1–10), transitional throacolumbar junction (T10–L2), and flexible lumbar spine (L3–5) [7]. This transition from the rigid thoracic spine with its link to ribs and sternum to the more mobile lumbar spine subjects the thoracolumbar region to significant biomechanical stress [5,8].
Neurological injuries quite often will further complicate the thoracolumbar junction fractures [9,10]. The probability of deficit in neurological function depends on the type of fracture. In a multicentric study, the occurrence of deficit of neurological function varied from 22% to 51% depending on the fracture type (22% in type A, 28% in type B, and 51% in type C fracture, according to the AO classification) [11].
Traditional classification protocols are described based on the morphology of the fracture, trauma mechanism, deficit of the neurological function, and damage to posterior ligamentous complex (PLC) [12]. There remains an absence of agreement on a few key areas such as indications for surgery and nonsurgical treatment of thoracolumbar fractures, as well as surgical stabilization’s superiority over conservative therapy for thoracolumbar burst fractures [13,14]. The World Federation of Neurosurgical Societies (WFNS), Spine Committee initiated this effort to formulate recommendations regarding the indications for surgery and nonsurgical treatment of thoracolumbar spine fractures through the published evidence and using elaborated methodology. Finally, these recommendations were formulated to improve patient care by defining the relevant literature and decision-making processes involved in the indications for surgical and nonsurgical treatment of thoracolumbar fractures. The surgical management of these patients often involves a multidisciplinary team. These recommendations were formulated as a guidance tool for surgeons through a series of indications for surgery and nonsurgical treatment of thoracolumbar spine fractures.
The systematic review and meta-analysis was conducted following the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines. The review followed the methods recommended by the Cochrane Handbook for Systematic Reviews of Interventions.
An international committee of spinal surgeons (members of the WFNS Spine Committee) organised a consensus meeting on the indications of surgical and nonsurgical management of thoracolumbar fractures. The meeting was conducted in Peshawar in December 2019 with WFNS Spine Committee members' presence and participation. The meeting aimed to analyze a preformulated questionnaire through preliminary literature review statements based on the current evidence levels to generate recommendations through a comprehensive voting session.
We utilized the Delphi method to administer the questionnaire to preserve a high degree of validity. To generate a consensus, the levels of agreement or disagreement on each item were voted independently in a blind fashion through a Likert-type scale from 1 to 5 (1=strongly disagree, 2=disagree, 3=somewhat agree, 4=agree, 5=strongly agree). Results were presented as a percentage of respondents who scored each item as 1 or 2 (disagreement) or as 3, 4, or 5 (agreement). The consensus was achieved when the sum for disagreement or agreement was ≥ 66%. Each consensus point was clearly defined with evidence strength, recommendation grade, and consensus level provided. The search strategy in the published protocol included studies on the indications for surgery and nonsurgical treatment of thoracolumbar spine fractures.
Articles were considered for review if they met the following inclusion criteria:
• Types of studies: randomized controlled trials, retrospective/prospective studies.
• Types of participants: patients who underwent conservative treatment for thoracolumbar spine fractures.
• Types of diagnosis: traumatic thoracolumbar spine fractures. Any osteoporotic thoracolumbar fractures were excluded.
• Types of treatments: nonoperative treatments.
• Outcomes: pain evaluation via visual analogue score (average VAS score), radiological features (mean kyphotic angle), loss in vertebral height (%), quality of life (36-item Short Form Health Survey [SF-36]), evaluated via physical compartment score, mental score, return to working life (days), length of hospital stay (days).
The electronic databases of PubMed, MEDLINE, and the CENTRAL (Cochrane Central Register of Controlled Trials), were searched from 2010 till 2020. A highly sensitive search strategy based on the Cochrane Handbook recommendations for Systematic Reviews of Interventions, combined with medical subject headings and keywords to identify potential articles, was employed. The search strategy was compiled in consultation with members of WFNS Spine Committee. In addition to the electronic database search, coauthors manually checked the list of references eligible trials and previous reviews. The complete search strategy is available.
The coauthors initially screened titles and abstracts of all records after duplicates were removed. The full-text article for each potentially eligible article was screened.
The coauthors independently used a standardized data extraction form to collate study characteristics (publication year, country, diagnosis [fracture type + neurological deficit], number of patients), type of intervention (nonoperative). Studies published induplicate were only included once.
The panel was asked to vote on the indications for nonsurgical treatment of thoracolumbar fractures. A total of 6 statements were drafted and voted in Peshawar in December 2019.
Publication date from 2010 to 2020; English language; main word search in all-fields: “thoracolumbar” “fractures” and “treatment” We obtained 1,264 articles across all databases, and after removing duplicates, we were left with 504 articles. Four hundred fifty papers (nonrelated) after abstract review by an independent double-check up were excluded. Following a full-text review of the remaining 54 studies, the authors selected 9 studies that met the inclusion criteria to draw conclusions (Fig. 1). Out of 17 studies, 4 were randomized controlled trials, and rest were retrospective.
Excluded studies included studies published in any language other than English, any case reports, animal studies, experimental studies, studies on osteoporotic thoracolumbar spine fractures, studies solely investigating surgical treatments.
Below is the review summary from those studies comparing nonoperative and operative treatment in AO type A fractures.
This review discusses guidelines and highlights the lack of high-level evidence studies regarding the indications for nonsurgical versus surgical treatment of traumatic thoracolumbar spine fractures. Several spinal fracture studies contain a high level of heterogeneity in the studied populations, including the spinal levels (mixed cervical and thoracolumbar and lumbar), mechanism of trauma, anatomical classification of trauma, surgical approaches performed as well as follow-up periods.
Fracture stability (comprised of mechanical and neurological stability) is a significant variable in formulating the therapeutic plan.
Denis [23] in 1983 first classified instability into 3 subgroups, mechanical instability, neurological instability, and the combined instability. The mechanical stability of the thoracolumbar spine is analyzed based on the integrity of the bony structures and the integrity of the posterior ligament complex [24-26]. On plain radiographs, reduction in the vertebral body height (50%), increased interspinous distance, and greater than 30°–35° of kyphotic deformity are indicators of injury to the posterior ligament complex [27-29]. Computed tomography (CT) could be used for evaluating diathesis of facet joints [30,31]. Magnetic resonance imaging is regarded as the most crucial examination in formulating the therapeutic plan for a patient with suspected PLC injury as it can analyze the PLC directly [32-34].
Neurological symptoms caused by a traumatic spinal injury can be classified with the Frankel scale or American Spinal Injury Association scale. Involvement of individual nerve root is categorized as Frankel grade E [35]. Apart from grade E, the other grades of thoracolumbar spine fracture with a complete or incomplete deficit of neurological function due to the role of spinal canal compromise are considered unstable fractures, irrespective of the instability from fracture itself or injury to the posterior element. Despite the above, fractures accompanied with the neurological deficit are not necessarily an absolute indication for surgery [36-39]. The surgical treatment is commonly conducted for cases with an incomplete neurological function deficit. It prevents further progression of neurological injury, aids in neurological recovery, and makes early mobilization possible by attaining fracture stability. However, if cases have Frankel A paralysis with complete neurological injury, the neurological exam should be conducted again after the period of spinal shock. If the neurological status is not changed on the second examination, there is a slim chance of neurological recovery expected due to decompression surgery [40]. Hence, the treatment aims to restore spinal alignments and fracture stabilization, resulting in faster mobilization and improved rehabilitation options and results [35,41].
Since the first sophisticated classifications introduced by Holdsworth in 1962 and by Denis in 1983, several classification systems have been formulated to aid in better communication among physicians, determine therapeutic strategies, and analyze the prognosis. Among such classification systems, McAfee classification, AO classification, and the thoracolumbar injury classification and severity score (TLICS) classification are most frequently utilized (Table 3) [12,23,24,27,42-54].
The mainstay of the thoracolumbar spine trauma management is based on modern comprehensive and easily reproducible classification that is based on:
• Objective clinical and imaging assessment.
• Provide standardized grading of the trauma.
• Identify any type of injury.
• Facilitates the decision if the fracture is stable/unstable.
• It gives the treatment direction – to fix or not to fix.
• Easily reproducible and easy to use in everyday practice.
Unfortunately, we are still searching for the ideal classification that will comply in 100% of the cases with the above criteria.
Oner et al. [55] and Wood et al. [50] indicated that the Denis classification system showed higher interobserver reliability than the AO classification system. Lenarz et al. [56] reported the comparison of Denis, AO, TLICS systems in 97 thoracolumbar fractures and observed that changes in reliability were present in all 3 scenarios, with the highest reliability happening in the senior resident cohort and attending spine surgeon cohort [56]. The lowest reliability was in the nonspine attending orthopedic and junior residents. In each cohort, the neurological function had the highest interobserver and intraobserver reliability. The researchers concluded that the TLICS is considered a widely deemed reliable tool compared to Denis and AO classification systems [57-59].
The goal of the management of thoracolumbar fractures involves reinstating the structural integrity and stability of the damaged spine, thus providing a biomechanically optimum environment for helping recovery. Historically, thoracolumbar fractures were managed primarily nonoperatively. However, recent technological improvements have shifted the transition from nonoperative to surgical treatment. However, the neurological deficit is seldom observed in cases managed nonoperatively. There is a lack of high-quality comparative research papers, with literature not confirming surgical treatment’s superiority over nonoperative treatment regarding pain management and restoration of neurological function [60-63].
Surgical treatment is seldom suggested for compression fractures. However, a vast proportion of flexion-distraction/fracture dislocations require surgery (stabilization). As surgical treatment is frequently recommended for thoracolumbar fractures with neurological deficits, the current review's main focus is the surgical management of fractures with neurological systems intact. To date, there is no high-quality, randomized research study supporting the superiority of surgical treatment over conservative treatment when there is no deficit of neurological function. Siebenga et al. [64] revealed that AO type A fractures (with an intact neurological system) treated by surgical treatment compared to nonoperative treatment revealed superior radiological results; however, clinical outcomes were similar [64].
Literature suggests that conservative treatment is indicated even in burst fractures with canal encroachment in the absence of a neurologic function's major deficit. The spinal canal’s spontaneous remodelling is one of the variables favouring nonoperative management [65].
In a spinal cord injury case, trauma to the neural structures happens both at the time of the trauma (primary – nonmodifiable) and in the subsequent period due to vascular dysfunction, edema, ischemia, electrolyte shifts, production of free radical, inflammation, and delayed apoptotic cell death (secondary – potentially modifiable) or iatrogenic reasons [68]. During prehospital treatment and in the emergency department management, also follow-up care, all the necessary measures should be taken to immobilize spinal trauma patients safely, to avoid a focal neurological deficit [12].
The statistics suggest that the majority of thoracolumbar fractures are stable, amenable to nonoperative management. The aim of nonoperative treatment is an appropriate regime of immobilization and, as early as possible, ambulation of the patient [69]. At the start, a short duration of bed rest may be indicated. Successful nonoperative treatment is based on patient collaboration, physiotherapists, nurses, and senior physicians. A change in treatment plan may be considered in the event of significant deterioration of clinical or radiological presentation [42].
Half of the thoracolumbar fractures are classified as compression type due to axial compression alone or flexion forces and present with wedge deformities of the vertebral body on radiological evaluation. Patients with compression-type fractures are seldom treated operatively as they are rarely associated with a current or potential deficit of neurological function [43].
Various pharmacological therapies are thought to alleviate secondary trauma have been studied in depth. These include steroids (anti-inflammatory), gangliosides, naloxone (opiate receptor blocker), calcium channel blockers, free radical scavengers, and neurotropic agents. Steroids were used quite heavily in the clinical management of spinal cord injury since mid of the 1960s. In animal spinal cord injury models, neurological recovery improved following steroid use [70]. After encouraging outcomes via an elevated dose of steroids in NASCIS (National Acute Spinal Cord Injury Study) 1 and 2 trials. However, in a third study, methylprednisolone failed to demonstrate an effect in comparison to placebo. Additionally, due to increased risk of infections, its use is no longer recommended [71]. American Association of Neurological Surgeons/Congress of Neurological Surgeons guidelines state that administration of methylprednisolone is no longer recommended as there is no class 1 or 2 study that has shown benefits. Hurlbert reported that the utility of high-dose methylprednisolone in the therapy of acute spinal cord injury is not proven as a standard of patient care [72]. A survey (2006) indicated that most of the respondents continue to give methylprednisolone, but by fear of litigation. However, in the current times, a high dose of steroid treatment is not considered to be a mainstream treatment [73].
Bracing is no longer considered necessary for the treatment of fractures of the vertebral column. Independent randomized control trials revealed no advantages from wearing braces [21,22]. In a systematic review, Giele et al. [74] reported that there is no evidence for the efficacy of bracing in cases with traumatic thoracolumbar fractures.
Literature regarding pain improvement from nonoperative and operative management of AO type A fractures is conflicted. A randomized prospective study evaluating stable burst fracture management revealed a statistically significant pain improvement from nonoperative treatment compared to surgical intervention [14]. Similar results were revealed by a large-scale retrospective study (n=230). However, the difference was not statistically significant [17]. On the other hand, Karaali et al. [15] evaluating compression, burst fractures (without neurological deficit) revealed that surgical management might yield a superior pain improvement in comparison to nonoperative management.
During conservative care, it is common to oversee a certain degree of increasing fracture kyphosis in most patients, frequently closer to the pretreatment sagittal alignment. However, kyphosis has not been showcased to link with increased pain levels in various studies, even up to 30° [13,75,76].
Nonoperative management is less efficacious in decreasing kyphotic angle in comparison to surgical management. Karaali et al. [15] revealed that the nonoperative cohort’s kyphotic angle (at the final follow-up, 24 months) of 17.61° to be higher than the surgical cohort (p<0.001). Similar results were observed from a range of retrospective studies (Pehlivanoglu et al. [16] and Shen et al. [19]).
Furthermore, nonoperative management seemed less successful in halting the loss of vertebral height than surgical management. Karaali et al. [15] revealed that at all follow-ups (3 months, 6 months, and 24 months), the nonoperative cohort had a significantly higher (p<0.001) loss of vertebral height versus the surgical cohort. Similar results were reported by the other retrospective designed studies; however, the 2 cohorts’ differences were not statistically significant.
Shamji et al. [20] evaluated bracing and nonbracing cohorts, and results revealed bracing to not be significantly superior to nonbracing cohorts in limiting vertebral height loss.
Literature on which management leads to a higher quality of life is conflicted. Pehlivanoglu et al. [16] revealed that the surgical cohort had a higher mental and physical compartment score than nonoperative cohorts. In contrast, Wood et al. [14] demonstrated that nonoperative cohorts had a significantly higher mental and physical score versus the surgical cohort.
Studies evaluating bracing and nonbracing cohorts did not reveal any statistically significant results regarding improving quality of life [21].
Literature on length of hospital stay for compression/burst fractures (without neurological deficit) managed nonoperatively and surgically is conflicted and lacking. While Karaali et al. [15] revealed a shorter hospital stay for patients managed nonoperatively, Pehlivanoglu et al. [16] showed otherwise.
All studies revealed that surgical management leads to a faster return to work versus nonoperative management regarding returning to work.
Each section within these recommendations suggests areas of need for future high-quality studies. However, as an overall requirement, future research should try to analyze patients with thoracolumbar trauma separate from patients with cervical trauma to better clarify the most effective diagnostic and treatment ways for these patients in particular.
Ensuring the best indications for nonsurgical or surgical treatment for the patients sustaining thoracolumbar fractures remains crucial. However, the available literature is still not unanimous, and further research is necessary. Compression-type fractures and stable burst fractures are mostly managed conservatively. If there is significant vertebral body structural damage, kyphotic angulation, neurological deficit, spinal canal compromise, surgical treatment may be considered. AO types B, C fractures are to be treated primarily surgically. The majority of the AO type A fractures may be treated conservatively.
• AO types B and C fractures preferably should not be treated conservatively (strongly agree 16.7%, agree 66.7%, disagree 16.7%).
• AO types A2, A3, and A4 can be treated conservatively if there is no significant vertebral body collapse, significant kyphotic angulation, or canal compromise with neurological impairment (agree 100%).
• There is no clinical evidence that bracing for conservative treatment of thoracolumbar fractures will improve the outcome (agree 100%).
• Fracture dislocations and cases with significant instability (score ≥ 5 of TLISS classification) should preferably be operated (strongly agree 16.7%, agree 83.3%).
• For burst fractures with neurological deficits, surgical decompression and stabilization may be considered, although there is not enough scientific evidence to support that (strongly agree 16.7%, agree 66.7%, disagree 16.7%).
• Burst fractures without neurological deficits can be treated either with conservative or surgical techniques (strongly agree 16.7%, agree 83.3%).
Fig. 1.
PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) flow diagram of the review process.
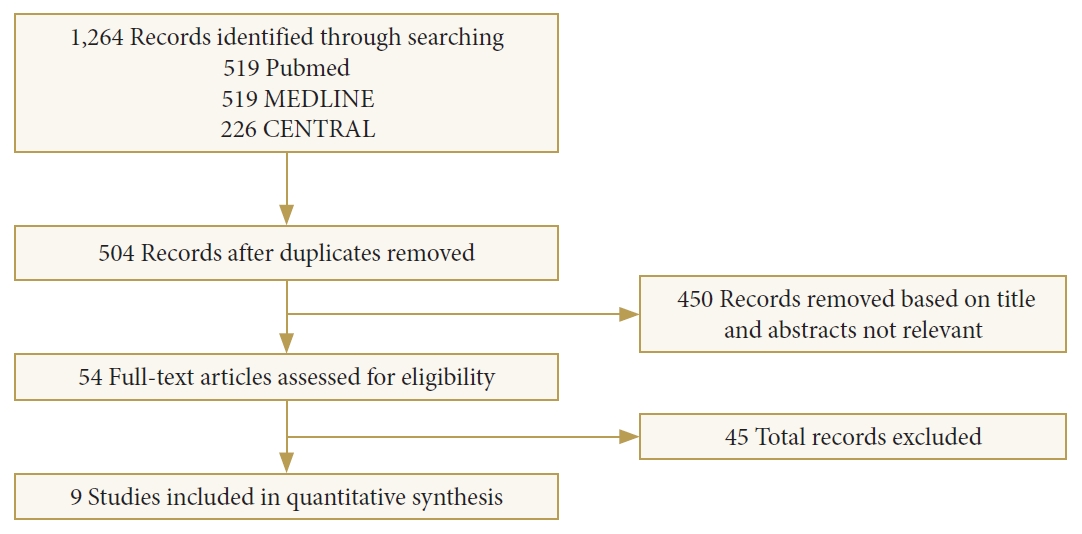
Table 1.
Clinical outcomes following nonoperative and operative treatments for AO type A thoracolumbar fractures
| Study | Study design | Country | No. | Fracture type + neurological deficit | Type of treatment | Mean pain score (VAS) | Mean kyphotic angle (°) | Mean vertebral height loss (%) | Mean physical compartment score (SF-36) | Mean mental compartment score (SF-36) | Mean hospital stay (day) | Mean return to work (day) |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Karaali et al. [15] (2020) | Retrospective | Turkey | 74 | Compression + burst fractures | Nonoperative vs. surgery | Nonoperative, 2.64; surgery, 1.91 | Nonoperative, 35.5; surgery, 25.12 | Nonoperative, 62.9; surgery, 21.2 | N/A | N/A | Nonoperative, 1.50; surgery, 3.18 | Nonoperative, 142.2; surgery, 104.79 |
| No neurological deficit | ||||||||||||
| Pehlivanoglu et al. [16] (2020) | Retrospective | Turkey | 45 | A3, A4 burst fractures | Nonoperative vs. surgery | Nonopera- tive, 2.3; surgery, 1.9 | Nonoperative, 11.65; surgery, 4.09 | Nonoperative, 12.78; surgery, 7.87 | Nonoperative, 56.67; surgery, 56.74 | Nonoperative, 55.5; surgery, 55.47 | Nonoperative, 11.0; surgery, 9.0 | N/A |
| No neurological deficit | ||||||||||||
| Nataraj et al. [17] (2018) | Retrospective | Canada | 230 | Burst fractures + no neurological deficit | Nonoperative vs. surgery | Nonopera- tive, 2.9; surgery, 3.3 | N/A | N/A | N/A | N/A | N/A | Nonoperative, 11.0; surgery, 23.0 |
| Urquhart et al. [21] (2017) | Randomized controlled trial | Canada | 96 | A3 fractures (burst) + no neurological deficit | TLSO (Brace) vs. no bracing | N/A | N/A | N/A | TLSO, 46.5%; no bracing, 45.5% | TLSO, 55.8%; no bracing, 55.2% | N/A | N/A |
| Hitchon et al. [18] (2016) | Retrospective | USA | 68 | Burst | Nonoperative vs. surgery | Nonopera- tive, 1.9; surgery, 3.0 | N/A | N/A | N/A | N/A | N/A | N/A |
| No deficit | ||||||||||||
| Shen et al. [19] (2015) | Retrospective | China | 129 | Burst + no (new) neurological deficit | Nonoperative vs. surgery | N/A | Nonoperative, 11.3; surgery, 22.7 | Nonoperative, 29.4; surgery, 31.5 | N/A | N/A | N/A | N/A |
| Wood et al. [14] (2015) | Prospective randomised | USA | 47 | Stable burst fracture | Nonoperative vs. surgery | Nonopera- tive, 1.5; surgery, 3.0 | N/A | N/A | Nonoperative, 89.5; surgery, 70.0 | Nonoperative, 89.0; surgery, 72.0 | N/A | N/A |
| No neurological deficit | ||||||||||||
| Shamji et al. [20] (2014) | Randomized controlled trial | Canada | 23 | Burst | Bracing (TLSO) vs. no bracing | N/A | N/A | TLSO, 47.6%; no bracing, 44% | TLSO, 51.6%; no bracing, 51.2% | TLSO, 43.3%; no bracing, 46.6% | N/A | N/A |
| No neurological deficit | ||||||||||||
| Bailey et al. [22] (2014) | Randomized equivalence trial | Canada | 47 | Burst | Orthoses vs. no orthoses | N/A | N/A | N/A | TLSO, 39.1%; no bracing, 36.6% | TLSO, 52.2%; no bracing, 50.8% | N/A | N/A |
| No neurological deficit |
Table 2.
A comparative analysis between nonoperative versus operative treatments for AO type A thoracolumbar fractures
Table 3.
The major characteristics and pros/cons of each classification system being used in evaluating thoracolumbar spine fractures
| Classification system | Characteristics | Pros/cons |
|---|---|---|
| Denis | 1. A 3-column theory based on 2-column theory of Holdsworth [24] | Pros: It is simple and introduces the idea of damage to the neurological system [43] |
| 2. Suggests that fractures of the middle column were very unstable. | Cons: it is quite challenging to identify thoracolumbar stable and unstable burst fractures [44] and interobserver reliability is low. | |
| 3. According to morphology of the fracture and mechanism of injury, thoracolumbar fractures were classified as compression, burst, flexion-distraction, and fracture dislocation. | Furthermore, it does not allow physicians to assess their therapeutic options for special fracture patterns on numerical evaluation of postfracture stability [45] | |
| McAfee | 1. PLC is a significant structure for the stability of the fracture, owing to the CT results. | Pros: Clear picture on surgical intervention required for type of fractures – stable burst or unstable burst [45] |
| 2. Subcategorised the middle column trauma and suggested that the middle column fails by a trio of several forces such as axial compression, distraction, and translation. | ||
| 3. Taking the mechanism of trauma into account, the authors separated such fractures into various categories, wedge compression fractures, stable, unstable burst fractures, chance fractures, flexion-distraction injuries, and translational injury [27] | Cons: lack of studies evaluating its reliability and validity [44] | |
| McCormack | 1. Forecasts the risk of failure of implant post posterior short-segment fixation for thoracolumbar spine fractures. | Pros: Load sharing score links well with the degree of spinal instability [46] |
| 2. Primarily introduction was in the aim of avoiding repeat kyphosis and failure of posterior short-segment fixation with pedicle screws through allowing the most suitable approach regarding approach (surgery). | Excellent inter- and intraobserver reliability was noted for junior surgeons [47] | |
| Cons: This classification intends only to identify fractures that would require additional anterior fixation following a posterior surgery [48] | ||
| AOSpine | 1. Categorises trauma into 3 groups, A (compression), B (distraction), and C (translation) injuries [49] taking into account mechanism of trauma, morphology of the fracture, and mechanical stability. | Cons: AO Classification attempted to advise the comprehensive classification including all varied type of fractures, it showcased solely moderate intraobserver and interobserver reliability owing to its complexity [44,50,51] |
| 2. Each category was further subcategorised from A1 to C3 (the higher the subgroup, the higher the severity of trauma and more unstable fractures | Further drawbacks include its inability to formulate a definition of stability of the fracture as well as no mention of a injury to the neurological function [43] | |
| TLICS | 1. The classification appears more comprehensive in comparison to the previous AO classification and includes information on neurological status and posterior ligamentous integrity [12] | Pros: The classification appears more comprehensive in comparison to the previous AO classification and includes significant information on neurological status and posterior ligamentous integrity [12] |
| 2. In terms of neurological functional status, grades vary from N0 (Neurologically intact), N1 (Transient deficit of neurological function), N2 (radicular symptoms), N3 (incomplete SCI or cauda equina injury), N4 (complete SCI), NX (unknown neurologic status owing to sedation or trauma to the head) [49] | ||
| 3. Morphological analyzes hold a great deal of significance as it aids in therapeutic choices [23] and categories vary from MM1 (abnormal alignment of vertebral column), MM2 (comminution of the vertebral body), MM3 (stenosis of the spinal canal), MM4 (intervertebral disc lesion). [42] The complete score was counted by talling up the scores from each of the 3 categories, and used to decide which treatment is most appropriate. | Evaluation of TLISS showcased fair to substantial intraobserver and interobserver reliability in various studies [52-54] | |
| 4. Conservative treatment is indicated for the total score of 3 points, 4 points to the grey area, where the decision on the therapy is taken by the physician, a score of 5 points indicates surgical treatment |
REFERENCES
1. Ghobrial GM, Jallo J. Thoracolumbar spine trauma: review of the evidence. J Neurosurg Sci 2013 57:115-22.

2. Ghobrial GM, Maulucci CM, Maltenfort M, et al. Operative and nonoperative adverse events in the management of traumatic fractures of the thoracolumbar spine: a systematic review. Neurosurg Focus 2014 37:E8.


3. Joaquim AF, Patel AA. Thoracolumbar spine trauma: Evaluation and surgical decision-making. J Craniovertebr Junction Spine 2013 4:3-9.



4. Katsuura Y, Osborn JM, Cason GW. The epidemiology of thoracolumbar trauma: a meta-analysis. J Orthop 2016 13:383-8.



5. Wood KB, Li W, Lebl DR, et al. Management of thoracolumbar spine fractures. Spine J 2014 14:145-64.


6. Dai LY, Yao WF, Cui YM, et al. Thoracolumbar fractures in patients with multiple injuries: diagnosis and treatment-a review of 147 cases. J Trauma 2004 56:348-55.


7. O’Toole JE, Kaiser MG, Anderson PA, et al. Congress of Neurological Surgeons systematic review and evidence-based guidelines on the evaluation and treatment of patients with thoracolumbar spine trauma: executive summary. Neurosurgery 2019 84:2-6.


8. el-Khoury GY, Whitten CG. Trauma to the upper thoracic spine: anatomy, biomechanics, and unique imaging features. AJR Am J Roentgenol 1993 160:95-102.


9. Magerl F, Aebi M, Gertzbein SD, et al. A comprehensive classification of thoracic and lumbar injuries. Eur Spine J 1994 3:184-201.


10. Kraemer WJ, Schemitsch EH, Lever J, et al. Functional outcome of thoracolumbar burst fractures without neurological deficit. J Orthop Trauma 1996 10:541-4.


11. Knop C, Blauth M, Bühren V, et al. Surgical treatment of injuries of the thoracolumbar transition 1: Epidemiology. Unfallchirurg 1999 102:924-35.

12. Rajasekaran S, Kanna RM, Shetty AP. Management of thoracolumbar spine trauma: an overview. Indian J Orthop 2015 49:72-82.



13. Wood K, Buttermann G, Mehbod A, et al. Operative compared with nonoperative treatment of a thoracolumbar burst fracture without neurological deficit. A prospective, randomized study. J Bone Joint Surg Am 2003 85:773-81.

14. Wood KB, Buttermann GR, Phukan R, et al. Operative compared with nonoperative treatment of a thoracolumbar burst fracture without neurological deficit: a prospective randomized study with follow-up at sixteen to twenty-two years. J Bone Joint Surg Am 2015 97:3-9.


15. Karaali E, Ciloglu O, Duramaz A, et al. Management of thoracolumbar injury classification and severity score of 4 (TLICS =4) thoracolumbar vertebra fractures: surgery versus conservative treatment. Ulus Travma Acil Cerrahi Derg 2020 26:805-10.

16. Pehlivanoglu T, Akgul T, Bayram S, et al. Conservative versus operative treatment of stable thoracolumbar burst fractures in neurologically intact patients: is there any difference regarding the clinical and radiographic outcomes? Spine (Phila Pa 1976) 2020 45:452-8.

17. Nataraj A, Jack AS, Ihsanullah I, et al. Outcomes in thoracolumbar burst fractures with a thoracolumbar injury classification score (TLICS) of 4 treated with surgery versus initial conservative management. Clin Spine Surg 2018 31:E317-21.


18. Hitchon PW, Abode-Iyamah K, Dahdaleh NS, et al. Nonoperative management in neurologically intact thoracolumbar burst fractures: clinical and radiographic outcomes. Spine (Phila Pa 1976) 2016 41:483-9.

19. Shen J, Xu L, Zhang B, et al. Risk factors for the failure of spinal burst fractures treated conservatively according to the thoracolumbar injury classification and severity score (TLICS): a retrospective cohort trial. PLoS One 2015 10:e0135735.



20. Shamji MF, Roffey DM, Young DK, et al. A pilot evaluation of the role of bracing in stable thoracolumbar burst fractures without neurological deficit. J Spinal Disord Tech 2014 27:370-5.


21. Urquhart JC, Alrehaili OA, Fisher CG, et al. Treatment of thoracolumbar burst fractures: extended follow-up of a randomized clinical trial comparing orthosis versus no orthosis. J Neurosurg Spine 2017 27:42-7.


22. Bailey CS, Urquhart JC, Dvorak MF, et al. Orthosis versus no orthosis for the treatment of thoracolumbar burst fractures without neurologic injury: a multicenter prospective randomized equivalence trial. Spine J 2014 14:2557-64.


23. Denis F. The three column spine and its significance in the classification of acute thoracolumbar spinal injuries. Spine (Phila Pa 1976) 1983 8:817-31.


24. Holdsworth F. Fractures, dislocations, and fracture-dislocations of the spine. J Bone Joint Surg Am 1970 52:1534-51.


25. Vaccaro AR, Zeiller SC, Hulbert RJ, et al. The thoracolumbar injury severity score: a proposed treatment algorithm. J Spinal Disord Tech 2005 18:209-15.

26. Terk MR, Hume-Neal M, Fraipont M, et al. Injury of the posterior ligament complex in patients with acute spinal trauma: evaluation by MR imaging. AJR Am J Roentgenol 1997 168:1481-6.


27. McAfee PC, Yuan HA, Fredrickson BE, et al. The value of computed tomography in thoracolumbar fractures. An analysis of one hundred consecutive cases and a new classification. J Bone Joint Surg Am 1983 65:461-73.


28. Benson DR, Burkus JK, Montesano PX, et al. Unstable thoracolumbar and lumbar burst fractures treated with the AO fixateur interne. J Spinal Disord 1992 5:335-43.


29. Reid DC, Hu R, Davis LA, et al. The nonoperative treatment of burst fractures of the thoracolumbar junction. J Trauma 1988 28:1188-94.


30. Schweitzer KM, Vaccaro AR, Harrop JS, et al. Interrater reliability of identifying indicators of posterior ligamentous complex disruption when plain films are indeterminate in thoracolumbar injuries. J Orthop Sci 2007 12:437-42.


31. Lee JY, Vaccaro AR, Schweitzer KM Jr, et al. Assessment of injury to the thoracolumbar posterior ligamentous complex in the setting of normal-appearing plain radiography. Spine J 2007 7:422-7.


32. Brightman RP, Miller CA, Rea GL, et al. Magnetic resonance imaging of trauma to the thoracic and lumbar spine. The importance of the posterior longitudinal ligament. Spine (Phila Pa 1976) 1992 17:541-50.


33. Emery SE, Pathria MN, Wilber RG, et al. Magnetic resonance imaging of posttraumatic spinal ligament injury. J Spinal Disord 1989 2:229-33.


34. Petersilge CA, Pathria MN, Emery SE, et al. Thoracolumbar burst fractures: evaluation with MR imaging. Radiology 1995 194:49-54.


35. Vaccaro AR, Lim MR, Hurlbert RJ, et al. Surgical decision making for unstable thoracolumbar spine injuries: results of a consensus panel review by the Spine Trauma Study Group. J Spinal Disord Tech 2006 19:1-10.

36. Andreychik DA, Alander DH, Senica KM, et al. Burst fractures of the second through fifth lumbar vertebrae. Clinical and radiographic results. J Bone Joint Surg Am 1996 78:1156-66.


37. Dai LY, Jiang LS, Jiang SD. Conservative treatment of thoracolumbar burst fractures: a long-term follow-up results with special reference to the load sharing classification. Spine (Phila Pa 1976) 2008 33:2536-44.

38. Knight RQ, Stornelli DP, Chan DP, et al. Comparison of operative versus nonoperative treatment of lumbar burst fractures. Clin Orthop Relat Res 1993 293:112-21.

39. Moller A, Hasserius R, Redlund-Johnell I, et al. Nonoperatively treated burst fractures of the thoracic and lumbar spine in adults: a 23- to 41-year follow-up. Spine J 2007 7:701-7.


40. Bohlman HH, Freehafer A, Dejak J. The results of treatment of acute injuries of the upper thoracic spine with paralysis. J Bone Joint Surg Am 1985 67:360-9.


41. Pneumaticos SG, Triantafyllopoulos GK, Giannoudis PV. Advances made in the treatment of thoracolumbar fractures:current trends and future directions. Injury 2013 44:703-12.


42. Verheyden AP, Spiegl UJ, Ekkerlein H, et al. Treatment of fractures of the thoracolumbar spine: recommendations of the spine section of the german society for orthopaedics and trauma (DGOU). Global Spine J 2018 8(2 Suppl):34S-45S.



44. Bono CM, Vaccaro AR, Hurlbert RJ, et al. Validating a newly proposed classification system for thoracolumbar spine trauma: looking to the future of the thoracolumbar injury classification and severity score. J Orthop Trauma 2006 20:567-72.


46. Wang XY, Dai LY, Xu HZ. The load sharing classification of thoracolumbar fractures: an—biomechanical validation. Spine 2007 32:1214-9.


47. Dai LY, Jin WJ. Interobserver and intraobserver reliability of the Load Sharing Classification in the assessment of thoracolumbar burst fractures. Spine 2005 30:354-8.


48. McCormack T, Karaikovic E, Gaines RW. The load sharing classification of spine fractures. Spine (Phila Pa 1976) 1994 19:1741-4.


49. Vaccaro AR, Oner C, Kepler CK, et al. AOSpine thoracolumbar spine injury classification system: fracture description, neurological status, and key modifiers. Spine (Phila Pa 1976) 2013 38:2028-37.

50. Wood KB, Khanna G, Vaccaro AR, et al. Assessment of two thoracolumbar fracture classification systems as used by multiple surgeons. J Bone Joint Surg Am 2005 87:1423-9.


51. Mirza SK, Mirza AJ, Chapman JR, et al. Classifications of thoracic and lumbar fractures: rationale and supporting data. J Am Acad Orthop Surg 2002 10:364-77.


52. Raja Rampersaud Y, Fisher C, Wilsey J, et al. Agreement between orthopedic surgeons and neurosurgeons regarding a new algorithm for the treatment of thoracolumbar injuries: a multicenter reliability study. J Spinal Disord Tech 2006 19:477-82.

53. Harrop JS, Vaccaro AR, Hurlbert RJ, et al. Intrarater and interrater reliability and validity in the assessment of the mechanism of injury and integrity of the posterior ligamentous complex: a novel injury severity scoring system for thoracolumbar injuries. Invited submission from the Joint Section Meeting On Disorders of the Spine and Peripheral Nerves, March 2005. J Neurosurg Spine 2006 4:118-22.

54. Patel AA, Vaccaro AR, Albert TJ, et al. The adoption of a new classification system: time-dependent variation in interobserver reliability of the thoracolumbar injury severity score classification system. Spine (Phila Pa 1976) 2007 32:E105-10.

55. Oner FC, Ramos LM, Simmermacher RK, et al. Classification of thoracic and lumbar spine fractures: Problems of reproducibility. A study of 53 patients using CT and MRI. Eur Spine J 2002 11:235-45.



56. Lenarz CJ, Place HM, Lenke LG, et al. Comparative reliability of 3 thoracolumbar fracture classification systems. J Spinal Disord Tech 2009 22:422-7.


57. Joaquim AF, de Almeida Bastos DC, Jorge Torres HH, et al. Thoracolumbar injury classification and injury severity score system: a literature review of its safety. Global Spine J 2016 6:80-5.


58. An Z, Zhu Y, Wang G, et al. Is the Thoracolumbar AOSpine Injury Score Superior to the thoracolumbar injury classification and severity score for guiding the treatment strategy of thoracolumbar spine injuries? World Neurosurg 2020 137:e493-8.


59. Yuksel MO, Gurbuz MS, Is M, et al. Is the thoracolumbar injury classification and severity score (TLICS) superior to the AO thoracolumbar injury classification system for guiding the surgical management of unstable thoracolumbar burst fractures without neurological deficit? Turk Neurosurg 2018 28:94-8.

60. Verlaan JJ, Diekerhof CH, Buskens E, et al. Surgical treatment of traumatic fractures of the thoracic and lumbar spine: a systematic review of the literature on techniques, complications, and outcome. Spine 2004 29:803-14.


61. van der Roer N, de Lange ES, Bakker FC, et al. Management of traumatic thoracolumbar fractures: a systematic review of the literature. Eur Spine J 2005 14:527-34.



62. Thomas KC, Bailey CS, Dvorak MF, et al. Comparison of operative and nonoperative treatment for thoracolumbar burst fractures in patients without neurological deficit: a systematic review. J Neurosurg Spine 2006 4:351-8.


63. Dai LY, Jiang SD, Wang XY, et al. A review of the management of thoracolumbar burst fractures. Surg Neurol 2007 67:221-31.


64. Siebenga J, Leferink VJ, Segers MJ, et al. Treatment of traumatic thoracolumbar spine fractures: a multicenter prospective randomized study of operative versus nonsurgical treatment. Spine 2006 31:2881-90.


65. Dai LY. Remodeling of the spinal canal after thoracolumbar burst fractures. Clin Orthop Relat Res 2001 382:119-23.

66. Vaccaro AR, Lehman RA, Hurlbert RJ, et al. A new classification of thoracolumbar injuries: the importance of injury morphology, the integrity of the posterior ligamentous complex, and neurologic status. Spine 2005 30:2325-33.


67. Tsou PM, Wang J, Khoo L, et al. A thoradic and lumbar spine injury severity classification based on neurologic function grade, spinal canal deformity, and spinal biomechanical stability. Spine J 2006 6:636-47.

68. Bunge RP, Puckett WR, Becerra JL, et al. Observations on the pathology of human spinal cord injury. A review and classification of 22 new cases with details from a case of chronic cord compression with extensive focal demyelination. Adv Neurol 1993 59:75-89.

69. Hides JA, Lambrecht G, Richardson CA, et al. The effects of rehabilitation on the muscles of the trunk following prolonged bed rest. Eur Spine J 2011 20:808-18.


70. Taoka Y, Okajima K, Uchiba M, et al. Methylprednisolone reduces spinal cord injury in rats without affecting tumor necrosis factor-alpha production. J Neurotrauma 2001 18:533-43.

71. Bracken MB, Shepard MJ, Holford TR, et al. Administration of methylprednisolone for 24 or 48 h or tirilazad mesylate for 48 h in the treatment of acute spinal cord injury. Results of the third national acute spinal cord injury randomized controlled trial ational acute spinal cord injury study. JAMA 1997 277:1597-604.


72. Hurlbert RJ. Methylprednisolone for acute spinal cord injury: an inappropriate standard of care. J Neurosurg 2000 93(1 Suppl):1-7.

73. Eck JC, Nachtigall D, Humphreys SC, et al. Questionnaire survey of spine surgeons on the use of methylprednisolone for acute spinal cord injury. Spine (Phila Pa 1976) 2006 31:E250-3.


74. Giele BM, Wiertsema SH, Beelen A, et al. No evidence for the effectiveness of bracing in patients with thoracolumbar fractures. Acta Orthop 2009 80:226-32.































