Comparative Analysis of 3 Types of Minimally Invasive Posterior Cervical Foraminotomy for Foraminal Stenosis, Uniportal-, Biportal Endoscopy, and Microsurgery: Radiologic and Midterm Clinical Outcomes
Article information
Abstract
Objective
The aim of this study was to compare the clinical and radiologic outcomes of 3 types of minimally invasive posterior cervical foraminotomy (PCF): uniportal endoscopic surgery, biportal endoscopic surgery, and microsurgery.
Methods
Between January 2019 to January 2020, PCF was performed using 3 different approaches to treat foraminal stenosis. The foraminal expansion rate, facet resection rate, and surgical foraminal approach angle were measured using magnetic resonance imaging. Visual analogue scale (VAS) scores for neck and arm pain, neck disability index (NDI), MacNab criteria, operation time, hospital stay, and complications were assessed. Clinical and radiologic parameters were compared among the 3 surgical groups.
Results
There were 38, 30, and 50 patients in the uniportal endoscopy, biportal endoscopy, and microscopy groups, respectively. Microscopy group displayed significantly higher foraminal expansion compared to uniportal endoscopy group (p=0.001). Facet resection rates and inclination angle for facet joint undercutting were significantly different among the 3 groups. Uniportal endoscopy group had the highest inclination angle and the least facet resection. On the 6 months and final follow-up, VAS scores and NDI were significantly lower in the uniportal endoscopy group than in the microscopy group (p=0.000).
Conclusion
All 3 types of PCF displayed favorable clinical outcomes and sufficient expansion of the midforaminal area. Two endoscopy groups showed a significantly higher inclination angle for undercutting the facet joint and a lower facet resection rate than the microscopy group. Reduced facet joint resection using an inclinatory approach did not interfere with sufficient foraminal expansion and enhanced the clinical result after 6 months of follow-up.
INTRODUCTION
Cervical radiculopathy is well known as a common spinal disease that leads to neck and arm pain, which is a typical manifestation of nerve root compression caused by intervertebral disc herniation or foraminal stenosis [1,2]. Surgical treatment should be considered when conservative management fails. Posterior cervical foraminotomy (PCF) has been reported to be effective for the treatment of cervical radiculopathy, as well as anterior cervical discectomy and fusion (ACDF) or disc replacement [1,3]. PCF has been performed using an open approach or via minimally invasive surgery (MIS) using a microscope or endoscopic system. A review of the literature revealed that both the open approach and MIS yield favorable clinical outcomes, but that MIS was superior to the open approach in terms of blood loss, operating time, and hospital stay [4-6]. Full endoscopic PCF has developed rapidly and has shown good clinical and radiological outcomes [7-10]. A meta-analysis by Wu et al. [11] revealed that both full endoscopic PCF and microscopic PCF offered equivalent clinical success rates, complication rates, and reoperation rates for cervical radiculopathy treatment. Recently, biportal endoscopic surgery has been widely performed with developed surgical techniques to treat cervical radiculopathy as well as central canal stenosis [12-14].
However, no study has compared the clinical outcomes or radiologic results characterizing the change of the foraminal space and facet joint among the 3 types of MIS PCF in a single center. In addition, there are few studies on whether endoscopic PCF can achieve complete neural decompression rates similar to microscopic PCF [15].
Therefore, the objective of this retrospective study was to compare the clinical and radiologic outcomes of 3 types of minimally invasive PCF: uniportal endoscopic surgery, biportal endoscopic surgery, and microsurgery.
MATERIALS AND METHODS
1. Study Patients
This study is a retrospective analysis of patients who underwent one of 3 types of minimally invasive PCF to treat radiculopathy due to foraminal stenosis between January 2019 and January 2020 at a single center. Five experienced spine surgeons performed all procedures. All 5 surgeons had more than 10 years of microscopic surgery experience and at least 5 years of uniportal endoscopic and biportal endoscopic surgery experience. The operative procedures were determined according to the experience and preferences of the operating surgeons. We provided information to the patients about each type of surgery before the operation. All patients who met the inclusion criteria were included in the study. All patients were followed up for 6–24 months, and data were collected during the follow-up period. All included patients met the following criteria:
(1) Presence of posterior neck pain, upper back pain, and radiating pain involving the upper extremities with a minimum of 6 weeks failed conservative treatment.
(2) Presence of radiculopathy due to foraminal stenosis at the unilateral side of a single cervical level confirmed by magnetic resonance imaging.
(3) Patients who had other accompanying asymptomatic foraminal stenosis in else to the operating lesion were included.
We excluded patients if they met any of the following criteria:
(1) The primary pathology was a foraminal soft herniated disc, and an additional discectomy was performed.
(2) Other cervical operations (decompression laminectomy, discectomy, multilevel foraminotomy, fusion, and total disc replacement) at different levels were performed simultaneously.
(3) Previous operation (ACDF, artificial disc replacement) at the index level.
(4) Accompanying segmental instability, symptomatic central stenosis, infectious disease, traumatic conditions, or musculoskeletal disorder.
2. Surgical Procedures
We performed 3 types of minimally invasive PCF: uniportal endoscopic PCF, biportal endoscopic PCF, and microscopic PCF. Each patient underwent surgery under general anesthesia in the prone position on a radiolucent Wilson frame for posterior surgery equipped with a chest bar. A compression-free sponge device was placed under the patient’s face, and the neck was slightly flexed. The slightly flexed neck position was maintained using skin tape without skull fixation. This was the same surgical position for all 3 different surgical approaches.
Microscopic PCF was performed using a tubular retractor system or a Caspar retractor (Aesculap Inc., Center Vally, PA, USA) with a microscope. A 2-cm longitudinal skin incision was made 1.5 cm lateral to the midline. A Kirschner (K)-wire was inserted carefully under fluoroscopic guidance and docked at the inferior-medial edge of the rostral facet joints of the involved level. Subsequently, serial dilators were inserted, with the final tubular retractor, measuring 16-mm or 18-mm in diameter, fixed on the targeted area using a retractor arm. After soft tissue removal, laminotomy and foraminotomy were performed using a high-speed drill and punches not to resect more than half of the facet joint. After confirming adequate nerve root decompression with a fine dissector, we completed the operation.
Uniportal endoscopic PCF cases utilized the interlaminar endoscopic system with an endoscope with a 12° viewing angle, an 8.4 mm outer diameter, 5.7-mm diameter working channel, and a 120-mm-long endoscope. A stab skin incision (8–10 mm) was made over the level of interest, targeting the medial border of the facet joint. The tissue dilator was passed through the underlying fascia, then the working cannula was inserted along the dilator under fluoroscopic guidance. The working cannula was docked on the lateral-most point of the 2-lamina covering the medial aspect of the facet joint. After soft tissue removal by coagulation with the radiofrequency probe, laminotomy and foraminotomy were performed using a 3.0-mm or 3.5-mm endoscopic drill. The foraminotomy was extended craniolaterally until the tip of the superior articular process (SAP) was exposed, then drilled laterally toward the lateral border of the lower-level pedicle for sufficient decompression of the distal foraminal part. During SAP drilling, the endoscope was tilted to obtain a broader inclinatory surgical view, seen craniolaterally to the SAP and lateral part of the foraminal area through a 12° endoscopic view angle. This surgical route with tilted endoscope facilitates reduction of the facet joint resection (Fig. 1A).
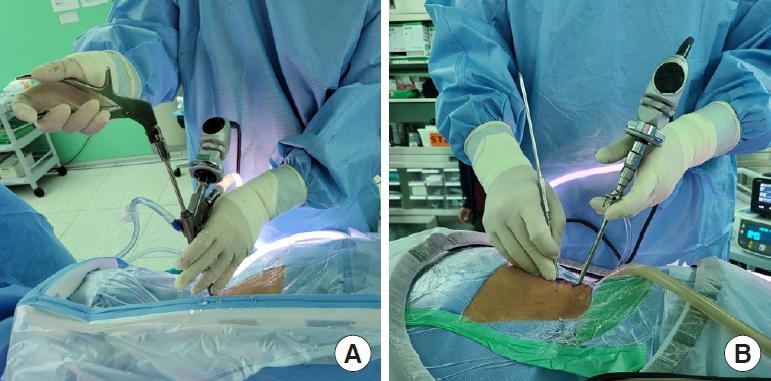
Intraoperative view of the uniportal endoscopic posterior cervical foraminotomy (A) and the biportal endoscopic posterior cervical foraminotomy (B).
Biportal endoscopic PCF cases utilized the usual biportal endoscopic systems with a 4.0-mm diameter, zero-degree optic view angle endoscope. Optimized fine surgical instruments, such as 1.0-mm and 2.0-mm Kerrison punch, and 1.5-mm pituitary forcep, were used. Two portals were made over the adjacent pedicles of the targeted level using serial dilators and a working sheath. The initial targeting area was also the medial border of the facet joint, and soft tissues were removed using a radiofrequency probe. The same laminotomy and foraminotomy procedures were performed using a 4.0-mm or 3.5-mm endoscopic diamond drill. The zero-degree endoscope and instruments accessed the lateral foraminal area in the mediolateral direction through the tilted portals to obtain the border foraminal surgical view and working space. Lateral part foraminotomy through the mediolaterally tilted surgical route was applied to reduce the facet resection (Fig. 1B).
3. Data Collection
This study was approved by the Ethics Committee of Leon Wiltse Memorial Hospital (NR-IRB 2021-W10). The requirement for informed consent was waived by the Ethics Committee due to the retrospective nature of the study. Information regarding patient characteristics, including age, sex, and clinical symptoms, was collected. Furthermore, the nature of the surgery, operation levels, operating time, and hospital stay were also documented, as were any postoperative complications. Surgeons and ward physicians collected the following information for each patient preoperatively, postoperatively, and at the 1-month, 6-month, and final follow-ups. Almost all patients were monitored using the above protocol after surgery, but those with complications were treated with additional management. Posterior neck and arm pain visual analogue scale (VAS) scores, neck disability index (NDI) scores, and MacNab criteria for evaluating disability and pain response were collected. A translation of 3 mm or more on a flexion-extension radiograph was considered to indicate instability [16].
4. Radiologic Parameters
We measured 4 parameters to characterize changes involving the foraminal space and the facet on the T2-weighted axial magnetic resonance (MR) images from the center of the operating intervertebral disc levels. Two values for the middle and distal foraminal widths and one for the facet length were measured. These values were measured pre- and postoperatively to evaluate changes in the operating structure. The measurement methods of Nakamura and Taguchi [15] were used to assess the facet length, distal foraminal width, and facet resection rate. We measured the facet drilling angle to characterize the surgical procedures of facet joint removal in 3 types of operations on the postoperative T2-weighted axial MR images, as described below.
(1) Midforaminal diameter (MFD): The shortest linear distance was measured on the line vertical to the longitudinal axis of the intervertebral foramen at the midforaminal part, and postoperative values were measured along the same plane (Fig. 2).

Measurement of 3 parameters on the T2-weighted axial magnetic resonance (MR) images from the operating intervertebral disc levels center. (A, B) Midforaminal diameter (A’), distal foraminal diameter (B’), and facet joint width (C’) were measured on the preoperative MR image. (C, D) Changes in the foraminal space and the facet joint were measured with 3 parameters; midforaminal diameter (C’), distal foraminal diameter (D’), and facet joint width (E’) was measured on the postoperative MR image from the same axial cut with preoperative measured level. (B, D) The measured point of the distal foraminal diameter in the facet joint medial border was 2-mm lateral from the outer margin of the uncovertebral joint.
(2) Distal foraminal diameter (DFD): The shortest linear distance was measured on the line vertical to the longitudinal axis of the intervertebral foramen at the distal foraminal part indicated 2 mm lateral from the outer edge of the vertebral body. Postoperative values were measured along the same plane (Fig. 2).
(3) Facet length (FL): The linear distance was measured between the medial and lateral borders of the facet joint from T2-weighted axial MR images of the middle of the facet joint.
(4) Surgical foraminal approach angle (SFAA): The angle was measured between 2 imaginary crossing lines. One was a line connecting the resected facet surface. The other line was parallel to the midline of the sagittal plane. We selected the axial cut of the MR image with the apparent facet resected surface for accurate measurement of the SFAA instead of the middisc level. A medial side acute angle to the sagittal plane indicated a negative value, and a lateral side acute angle indicated a positive value. Any negative values indicated an inclination angle through undercutting the facet (Fig. 3).
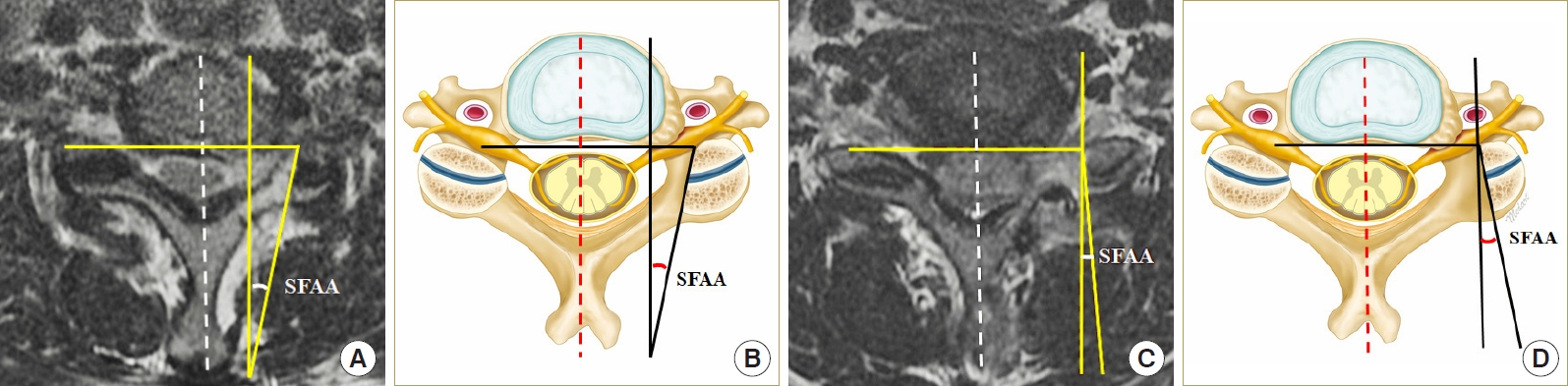
The surgical foraminal approach angle (SFAA) was measured to the facet joint on the postoperative T2-weighted axial magnetic resonance (MR) images. This angle was measured between 2 imaginary crossing lines, a line connecting the resected facet joint surface and a parallel line with the midline of the sagittal plane. The measured angle revealed either a negative value (A, B) or a positive value (C, D).
(5) Foraminal expansion rate: We calculated the expansion of the narrowed foraminal space after foraminotomy using the pre- and postoperative values of the MFD and DFD. The calculation formula was (
(6) Facet joint resection rate: We calculated the estimated amount of facet resection using the pre- and postoperative FL. The formula used was
5. Statistical Analysis
Statistical analysis was performed using PASW Statistics ver. 18.0 (SPSS Inc., Chicago, IL, USA). Continuous variables were expressed as means and standard deviations. Clinical VAS and NDI scores were measured preoperatively, postoperatively, and at the 1-month, 6-month, and final follow-ups, and MacNab criteria were assessed at the final follow-up, which was all reported by the patients and analyzed with paired t-tests. Analysis of variance and post hoc analysis were used to compare operation times, hospital stay lengths, and radiologic parameter values with outcomes among the 3 independent groups. The paired t-test assumed normality of distribution because the number of patients in each group was more than 30. A p-value of < 0.05 was considered to indicate a significant difference. The results of post hoc analysis were indicated.
RESULTS
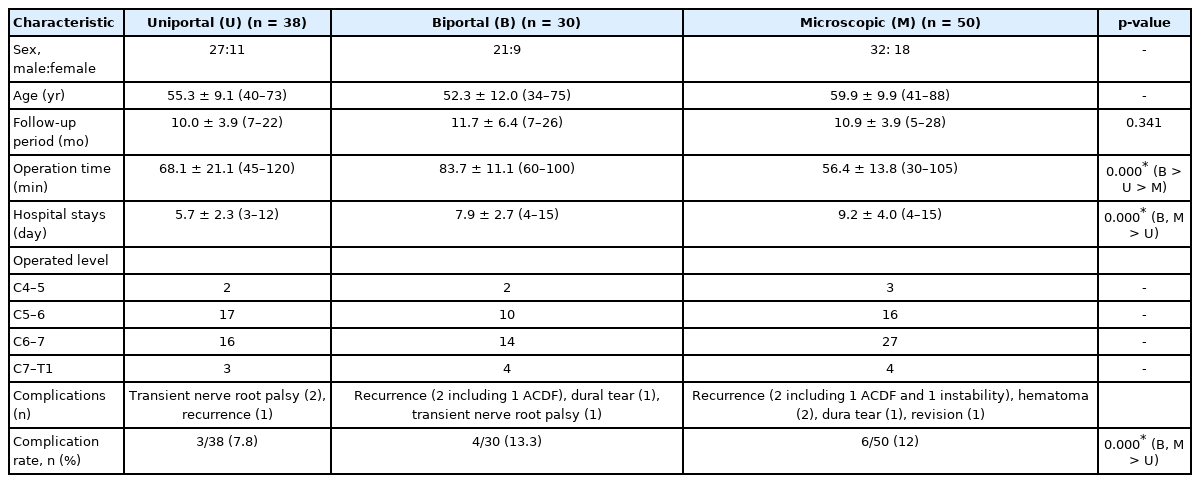
A total of 38 (27 men and 11 women), 30 (21 men and 9 women), and 50 (32 men and 18 women) patients who had undergone uniportal posterior endoscopic cervical foraminotomy (PECF), biportal PECF, and microscopic PCF, respectively, were included. The mean age was 55.3±9.1 years (range, 40–73 years) in the uniportal endoscopy group, 52.3±12.0 years (range, 34–75 years) in the biportal endoscopy group, and 59.9±9.9 months (range, 41–88 months) in the microscopy group (Table 1). The mean follow-up duration was 10.0±3.9 months (range, 7–22 months) in the uniportal endoscopy group, 11.7±6.4 years (range, 7–26 years) in the biportal endoscopy group, and 10.9±3.9 years (range, 5–28 years) in the microscopy group. There was no significant difference in follow-up duration among the 3 surgical groups (Table 1). Mean operating time in the microscopy group was significantly lower than that in the endoscopic surgical groups. Further, the uniportal endoscopy group had a significantly lower operating time than the biportal endoscopy group (microscopy: 56.4±13.8, uniportal endoscopy: 68.1±21.1, biportal endoscopy: 83.7±11.1, both p=0.000) (Table 1). The mean hospital stay in the uniportal endoscopy group was significantly lower than those in the biportal endoscopy or microscopy groups (uniportal endoscopy: 5.7±2.3, biportal endoscopy: 7.9±2.7, microscopy: 9.2±4.0, both p=0.000) (Table 1). The operated spinal levels were C4–5 (n=2), C5–6 (n=17), C6–7 (n=16), and C7–T1 (n=3) in the uniportal endoscopy group, C4–5 (n=2), C5–6 (n=10), C6–7 (n=14), and C7–T1 (n=4) in the biportal endoscopy group, and C4–5 (n=3), C5–6 (n=16), C6–7 (n=27), and C7–T1 (n=4) in the microscopy group (Table 1). The C5–6 and C6–7 levels were the most common operating levels among the 3 groups.
Surgery-related complications have occurred in all 3 surgical groups. There were 2 transient nerve root palsies and 1 recurrence case in the uniportal endoscopy group. In the 2 transient nerve root palsy cases, shoulder abduction weakness occurred after the C4–5 level operation, and hand grasp weakness was developed after the C6–7 level operation. The symptoms of nerve root palsy were recovered with 2 weeks of conservative treatment. One dural tear, 1 transient nerve root palsy, and 2 recurrence cases occurred in the biportal endoscopy group. Two postoperative hematomas, 1 dura tear, and 2 recurrences, including 1 case of segmental instability and 1 patient who underwent revision surgery due to postoperative arm weakness were noted in the microscopy group. We assessed detailed data for symptom-relapsed cases. One patient in the uniportal endoscopy group relapsed symptomatically at the 6-month follow-up due to insufficient decompression (expansion rate of MFD, 1.34; facet resection rate, 22.0%; SFAA, +10°). In the biportal endoscopy group, 1 patient underwent ACDF surgery at the 2-year follow-up due to insufficient foraminal enlargement (expansion rate of MFD, 1.37; facet resection rate, 28.6%; SFAA, +7.8°); another patient relapsed symptomatically after 3 months even with successful foraminal decompression but improved after conservative treatment (expansion rate of MFD, 3.25; facet resection rate, 47.6%; SFAA, -13.8°). In the microscopy group, 1 patient relapsed at the 2-month follow-up due to segmental instability and underwent ACDF surgery (expansion rate of MFD, 4.1; facet resection rate, 70.5%; SFAA, +0.5°). Another patient relapsed at the 1-year follow-up due to insufficient foraminal expansion (expansion rate of MFD, 2.4; facet resection rate, 35.3%; SFAA, +2.5°) and was treated with conservative management. The complication rate of the uniportal endoscopy group was significantly lower than that of the biportal endoscopy and microscopy groups (uniportal endoscopy, 7.8%; biportal endoscopy, 13.3%; microscopy group, 12%; both p=0.000) (Table 1).
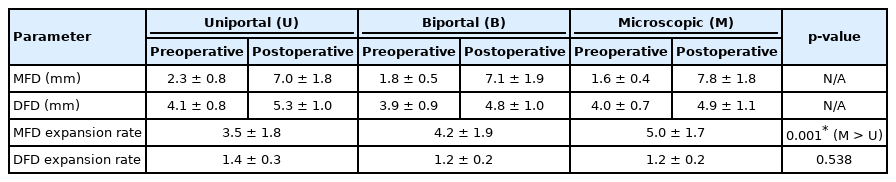
We measured the MFD and DFD to characterize the foraminal space and analyzed values focused on the changes, using the formula for the foraminal expansion rate. The mean expansion rate of MFD in the uniportal endoscopy group was 3.5±1.8 (preoperative MFD, 2.3±0.8 mm; postoperative MFD, 7.0±1.8 mm); in the biportal endoscopy group was 4.2±1.9 (preoperative MFD, 1.8±0.5 mm; postoperative MFD, 7.1±1.9 mm); and in the microscopy group was 5.0±1.7 (preoperative MFD, 1.6±0.4 mm; postoperative MFD, 7.8±1.8 mm) (Table 2). All surgical groups showed more than 3 times midforaminal expansion. The MFD expansion rate of the microscopy group was significantly higher than that of the uniportal endoscopy group (p=0.001) (Table 2). The mean expansion rate of DFD in the uniportal endoscopy group was 1.4±0.3 (preoperative DFD, 4.1±0.8 mm; postoperative DFD, 5.3±1.0 mm); in the biportal endoscopy group was 1.2±0.2 (preoperative DFD, 3.9±0.9 mm; postoperative DFD, 4.8±1.0 mm); and in the microscopy group was 1.2±0.2 (preoperative DFD, 4.0±0.7 mm; postoperative DFD, 4.9±1.1 mm). There was no significant difference regarding distal foraminal expansion among the 3 surgical groups (Table 2).
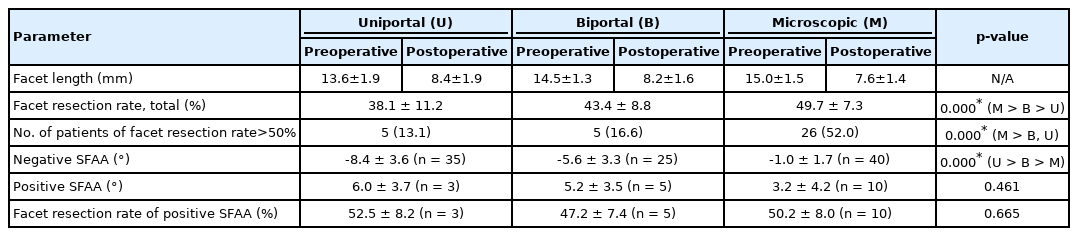
We measured the FL to characterize the facet and analyzed the values focused on the amount of facet resection using the formula for the facet resection rate. The total facet resection rate in the uniportal endoscopy group was 38.1%±11.2% (preoperative FL, 13.6%±1.9%; postoperative FL, 8.4%±1.9%); in the biportal endoscopy group was 43.4%±8.8% (preoperative FL, 14.5±1.3 mm; postoperative FL, 8.2±1.6 mm); and in the microscopy group was 49.7%±7.3% (preoperative FL, 15.0±1.5 mm; postoperative FL, 7.6±1.4 mm). The total facet resection rate was significantly higher in the microscopy group than in the 2 endoscopic surgical groups, and the biportal endoscopy group had a significantly higher facet resection rate than the uniportal endoscopy group (both p=0.000) (Table 3). Furthermore, the percentage of patients with more than 50% facet resection rate was significantly higher in the microscopy group than in the 2 endoscopy groups (microscopy, 52%; biportal endoscopy, 16.6%; uniportal endoscopy, 13.1%) (Table 3).
We tracked the surgical route through the resected facet and measured the tracked approach angle to the foraminal space using the SFAA. In addition, we analyzed the effect of SFAA on the pattern and amount of facet resection. The SFAA showed negative or positive values according to the direction of the surgical approach, medial to the lateral direction, or lateral to medial direction, respectively. Positive values were expected to correlate with more extensive facet resection, especially for the inferior articular process; therefore, we analyzed the facet resection rate in cases with positive SFAA values. The mean negative SFAA was -8.4°±3.6° (35 out of 38 patients) in the uniportal endoscopy group; -5.6°±3.3° (25 out of 30 patients) in the biportal endoscopy group; and -1.0°±1.7° (40 out of 50 patients) in the microscopy group (Table 3). The absolute values of negative SFAA in the 2 endoscopy groups were significantly higher than those in the microscopy group, and the uniportal endoscopy group showed a significantly higher angle than the biportal endoscopy group (both p=0.000) (Table 3).
According to the facet resection rate and SFAA, the lower absolute values of negative SFAA showed a higher facet joint resection rate. Positive SFAA seemed to be correlated with higher facet joint resection; hence, we calculated the facet resection rate in patients with positive SFAA to evaluate the correlation between the positive SFAA and excessive facet removal. The mean positive SFAA was 6.0°±3.7° (3 out of 38 patients) in the uniportal endoscopy group; 5.2°±3.5° (5 out of 30 patients) in the biportal endoscopy group; and 3.2°±4.2° (10 out of 50 patients) in the microscopy group. A significant difference was not found among the 3 surgical groups (p=0.461; Table 3). The facet resection rate of positive SFAA was 52.5°±8.2° in the uniportal endoscopy group, 47.2°±7.4° in the biportal endoscopy group, and 50.2°±8.0° in the microscopy group, showing a higher facet resection rate than in the negative SFAA patients for each surgical group. However, there was no significant difference in the facet resection rate with positive SFAA among the 3 surgical groups (p=0.665) (Table 3).
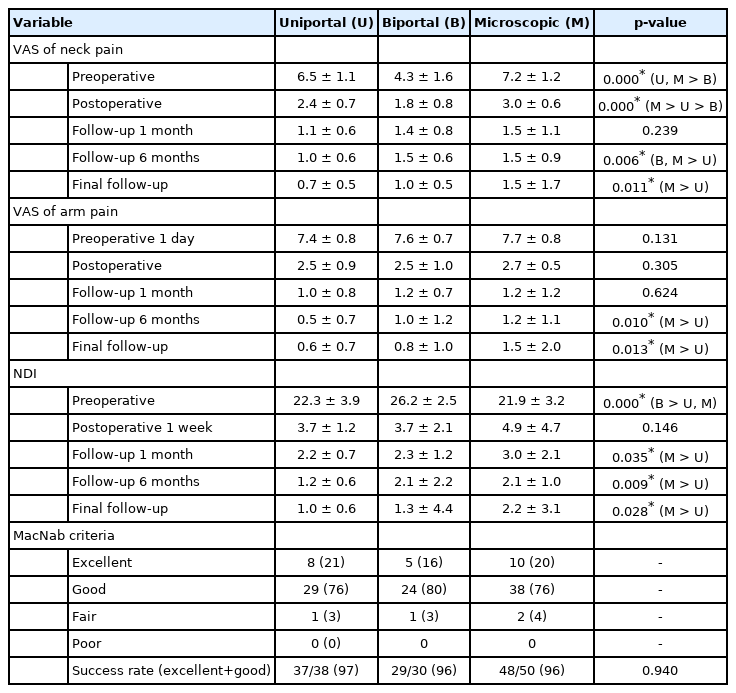
The VAS scores for neck and arm pain in the 3 surgical groups were significantly improved after surgery. The mean scores of uniportal endoscopy group preoperatively, and at 1 day (postoperative), 1 month, 6 months, and at the final follow-up were 6.5±1.1, 2.4±0.7, 1.1±0.6, 1.0±0.6, and 0.7±0.5, respectively for arm pain and were 7.4±0.8, 2.5±0.9, 1.0±0.8, 0.5±0.7, and 0.6±0.7, respectively, for neck pain. The mean VAS scores of biportal endoscopy group were 4.3±1.6, 1.8±0.8, 1.4±0.8, 1.5±0.6, and 1.0±0.5, respectively for arm pain and were 7.6±0.7, 2.5±1.0, 1.2±0.7, 1.0±1.2, and 0.8±1.0, respectively for neck pain. The mean VAS scores of microscopy group were 7.2±1.2, 3.0±0.6, 1.5±1.1, 1.5±0.9, and 1.5±1.7, respectively for arm pain, and were 7.7±0.8, 2.7±0.5, 1.2±1.2, 1.2±1.1, and 1.5±2.0, respectively for neck pain (p=0.000 in all groups and in all follow-ups) (Table 4, Fig. 4). There was no significant difference in neck pain VAS scores between the microscopy and uniportal endoscopy groups preoperatively; however, the uniportal endoscopy group showed significantly lower scores than the microscopy group postoperatively, and at the 6-month and final follow-ups (p=0.000, p=0.06, p=0.011, respectively). The uniportal endoscopy group had significantly higher preoperative neck pain VAS scores than the biportal endoscopy group; however, the inverse result was shown at the 6-month follow-up (Table 4). Significant differences in arm pain VAS scores were not observed among the 3 surgical groups preoperatively, postoperatively, and at 1 month; however, the uniportal endoscopy group showed significantly lower scores than the microscopy group at the 6-month and final follow-ups (p=0.010 and p=0.013, respectively) (Table 4).
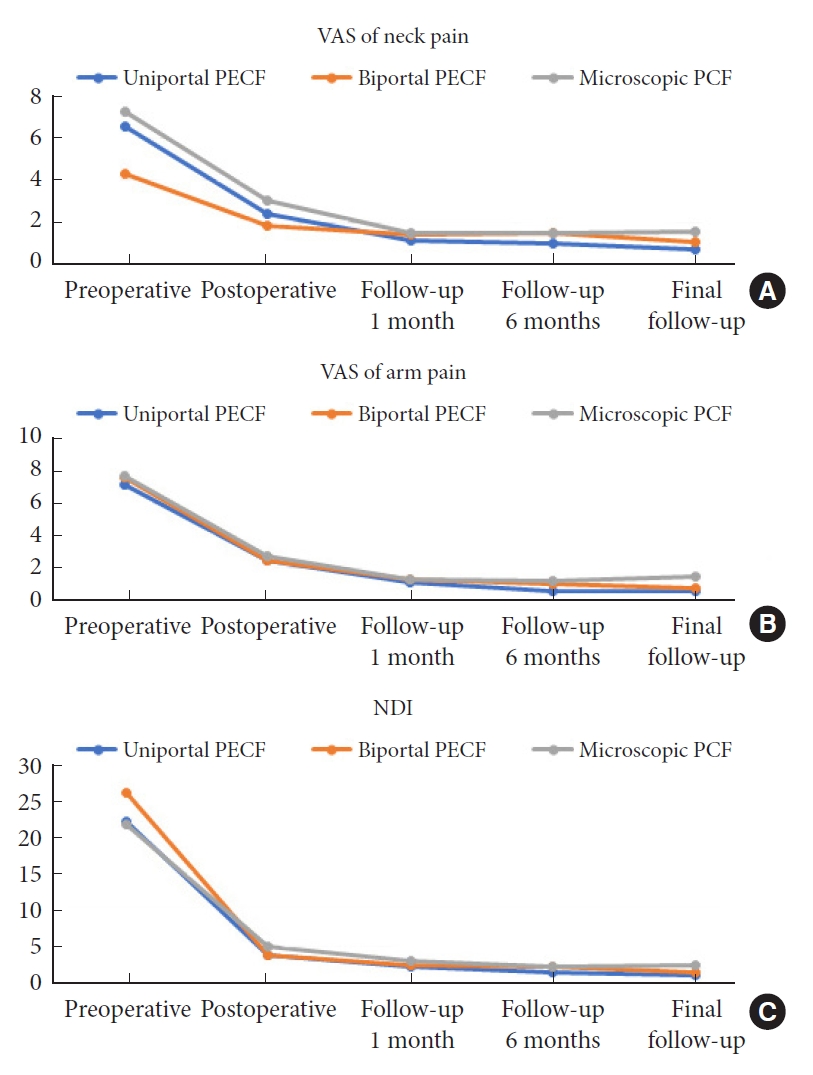
Clinical outcomes. Mean visual analogue score (VAS) of neck pain and arm pain (A, B), and neck disability index (NDI) (C) preoperatively and at postoperative, 1 month, 6 months, and final follow-up showed a clinically significant decrease (p=0.000 in VAS of neck pain and arm pain, p=0.000 in NDI, all follow-up period). A p-value of < 0.05 was considered to indicate a statistically significant difference. PECF, posterior endoscopic cervical foraminotomy; PCF, posterior cervical foraminotomy.
There was a significant improvement in the NDI scores. The mean scores preoperatively and at the 1 week, 1 month, 6 months, and final follow-ups were 22.3±3.9, 3.7±1.2, 2.2±0.7, 1.2±0.6, and 1.0±0.6, respectively, in the uniportal endoscopy group; 26.2±2.5, 3.7±2.1, 2.3±1.2, 2.1±2.2, and 1.3±4.4, respectively, in the biportal endoscopy group; and 21.9±3.2, 4.9±4.7, 3.0±2.1, 2.1±1.0, and 2.2±3.1, respectively, in the microscopy group (p=0.000 in all groups and all follow-up) (Table 4, Fig. 4). There was no significant difference in NDI scores between the microscopy and uniportal endoscopy groups preoperatively; however, the uniportal endoscopy group showed significantly lower scores than the microscopy group at the 1-month, 6-month, and final follow-ups (p=0.000, p=0.035, p=0.009, p=0.028, respectively) (Table 4).
MacNab criteria found that there were 7 (21%), 29 (76%), and 1 (3%) excellent, good, and fair outcomes in the uniportal endoscopy group, respectively; 5 (16%), 24 (80%), and 1 (3%) excellent, good, and fair outcomes in the biportal endoscopy group, respectively; and 10 (20%), 38 (76%), and 2 (4%) excellent, good, and fair outcomes in the microscopy group, respectively. There were no significant differences in the success rate among the 3 surgical groups (uniportal, 97%; biportal, 96%; microscopy, 96%; p=0.940) (Table 4).
DISCUSSION
Each of the 3 minimally invasive approaches has a characteristic surgical technique for successful cervical foraminal decompression. The different equipment and techniques used in the 3 types of PCF could influence the radiologic results of facet resection and foraminal expansion. Further, these radiologic features could affect the clinical results. Based on 3 approaches, we focused on characterizing the pattern and amount of facet resection, as well as the expansion of the mid and distal foraminal areas. We then closely analyzed whether radiologic features influenced the clinical results, such as symptom improvement, recurrence, and segmental instability, by comparing the 3 approaches.
1. Operating Time
Cervical paraspinal muscular structures consist of multiple layers of muscle and thick fascia. Thick fascia layers commonly interfere with the process of making portals in the uniportal and biportal endoscopic surgery. Two portals with different directions should be created through the multilayered fascia for the biportal endoscopic surgery, and the working portal can be obstructed by the flapping pieces of the fascia, although working sheath is used. Therefore, it may need more time to make 2 portals with the proper saline flow during the biportal endoscopic surgery in the cervical spine.
2. The Characteristics of Foraminal Expansion and Facet Joint Resection
Nerve root compression is predominantly observed at the entrance zone of the intervertebral foramen; however, foraminal stenosis extends to involve the exit zone in many cases. Generally, in PCF, the medial side of the facet joint is removed while preserving the lateral side by more than 50% since Zdeblick et al. [17] demonstrated that facet joint resection of > 50% causes segmental hypermobility. On resection of the facet joint ≤ 50%, any foraminal stenosis at the lateral edge of the resection area may not be sufficiently decompressed because of technical difficulties. Excessive facet violation is inevitable when resolving distal foraminal stenosis. This general principle applies to all 3 types of minimally invasive PCF; however, this study showed somewhat different radiologic results of facet joint resection and foraminal expansion depending on the approach.
All surgical groups showed more than 3 times expansion of the midforaminal part, but the expansion rate of the microscopy group (5.0±1.7) was significantly higher than in the uniportal endoscopy group (3.5±1.8; Table 2). However, VAS and NDI scores at the 6-month and final follow-ups showed better improvements in the uniportal endoscopy groups than in the microscopy group (Table 4). If the midforaminal area was expanded by approximately 3 times, this seemed to be enough to achieve sufficient neural decompression, and symptomatic improvement could be continued till the 1-year follow-up, with minimal relapse of symptoms. More extensive foraminal decompression in the microscopy group was not associated with better VAS and NDI scores than in the endoscopy group. Furthermore, almost all symptom recurrence cases were caused by insufficient midforaminal expansion or segmental instability, with only one patient relapsing symptomatically despite sufficient foraminal decompression (Table 1).
Expansion of the distal foraminal part was insignificant in all surgical groups. However, despite remaining stenosis in the distal foraminal part, all 3 groups showed significantly improved VAS and NDI scores in all follow-up periods after surgery. The remaining distal foraminal stenosis did not seem to affect postoperative clinical outcomes, which is consistent with a report by Nakamura et al. [15].
3. Facet Joint Resection Associated With Inclinatory Surgical Route
Adequate facet joint resection is necessary for sufficient nerve root decompression; however, the resection area is limited because of the risk of segmental instability. Zdeblick et al. [17] reported that instability slightly increased with a facet resection rate of up to 50%, but markedly increased with a facet resection rate of 75%. Chang et al. [18] and Song and Lee [12] reported that undercutting the facet joint via an inclinatory surgical route is essential in terms of preserving the facet joint and capsule [12,18], further reporting favorable clinical outcomes. The 2 endoscopy groups in this study utilized a higher inclination angle when undercutting the facet joint and subsequently preserved the facet joint better than the microscopy group. Moreover, the uniportal endoscopy group had a higher inclination angle and less facet joint resection than the biportal endoscopy group. These remarkable radiologic outcomes may be due to the endoscopic approach-related advantages of PCF.
Endoscopic systems used in the PCF place the surgeon’s vision within the operating space. Further, small-diameter endoscopy has fewer limitations for viewing of the foraminal space through the undersurface of the resected facet joint. With free movements of endoscopic views, adequate foraminal decompression can be achieved by undercutting the facet joint while preserving the facet joint and capsule through an inclinatory surgical route (Fig. 5). Furthermore, uniportal endoscopy with a 12° endoscopic view can reveal the deeper foraminal space even if the preserved facet joint interferes with the surgical viewing compared to biportal endoscopy with a zero-degree endoscopic view. Although biportal endoscopic and microscopic surgery can achieve cervical posterior inclinatory foraminotomy using the contralateral-sided endoscopic approach [12] and anterior cervical retractor system [18], respectively, ipsilateral-sided conventional surgeries might have less ability to make a higher inclinatory surgical route than uniportal endoscopic surgery. Making an inclinatory surgical route is challenging during microscopic PCF because the spinous process restricts the direction of resection, and almost all patients had a nearly vertical approach angle when using this technique (mean negative SFAA, -1.0°±1.7°). Furthermore, the facet joint is also resected in proportion to the extent of foraminal decompression due to the limited surgical corridor of microscopic surgery. Accordingly, in the microscopy group, 52% of patients showed facet joint resection of > 50%, and the proportion was significantly higher than in the 2 endoscopy groups (Table 3).

Illustrated cases of posterior cervical foraminotomy (PCF). (A, B) Postoperative magnetic resonance (MR) images showed the well-preserved facet joint (blue flower mark) and the surgical tracts of inclination angle for undercutting the facet joint (long yellow arrow). (C, D) Extensive facet joint resections were found (white flower mark) with surgical tracts of vertical or medial direction angle (long white arrow). Symptom-relapsed cases showed insufficient foraminal decompression (yellow flower mark) in both surgical routes of a medial direction angle (E, long white arrow) and an inclination angle (F, long yellow arrow).
Clinical results of VAS of neck pain, VAS of arm pain, and NDI showed remarkable improvements compared to their respective preoperative scores. However, when comparing the 3 surgical groups, somewhat different scores were shown after 6 months of follow-up. The uniportal endoscopy group had significantly lower VAS scores for neck and arm pain and NDI scores than the microscopy group at the 6-month and final follow-ups. This may be caused by having had the highest inclination angle and the least facet resection of any group. Furthermore, in the uniportal endoscopy group, less foraminal decompression than the microscopy group did not affect improvements in midterm VAS and NDI scores; instead, it seemed to enhance the clinical outcomes after 6 months of follow-up due to facet joint preservation.
The microscopy group showed a significantly higher proportion of facet resection (> 50%) than the 2 endoscopic groups, but just by a little more than 50%; among them, only 1 patient with 70.5% facet resection had segmental instability and underwent ACDF surgery. Furthermore, 13.1% of patients in the uniportal endoscopy group and 16.6% of patients in the biportal endoscopy group had facet resection of > 50% with no segmental instability occurring. It is assumed that resection by a little more than 50% does not cause problems with intervertebral stability [15]. Therefore, it seems better to prioritize sufficient facet joint removal over preservation for more favorable symptom improvement if the inclinatory foraminal approach is not applicable.
The present study has several limitations. This study was retrospective, and the follow-up period was relatively short. However, it was reasonable to assess the midterm results greatly affected by the natural course according to the 3 different surgical approaches. Although generally experienced surgeons aim to achieve sufficient foraminal decompression, determining the resection area could differ according to the surgeon’s propensity. Therefore, we cannot rule out the surgeon’s influence on radiologic outcomes. We measured facet joint resection using the linear distance, and this did not represent the total volume of the resected facet joint. Expansion of the foraminal diameter was measured at the most stenotic middisc level. This did not represent all foraminal changes.
Nonetheless, this study is important because it investigated midterm clinical outcomes, which were affected by the different radiologic results based on the features of 3 minimally invasive approaches. Furthermore, we analyzed the details of symptom-relapse cases. A multicenter study with a larger sample size and long-term follow-up is required to confirm the findings of the current study.
CONCLUSION
Three types of minimally invasive PCF revealed favorable clinical outcomes and sufficient expansion of the midforaminal area. The 2 endoscopy groups showed a significantly higher inclination angle for undercutting the facet joint and a lower facet resection rate than the microscopy group. Reduced facet joint resection using an inclinatory approach did not interfere with sufficient foraminal expansion and enhanced the clinical result after 6 months of follow-up.
Notes
Conflict of Interest
The authors have nothing to disclose.
Funding/Support
This study received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author Contribution
Conceptualization: JYK, HJH, DCL, CKP; Data curation: JYK, DCL, THK, JSH; Formal analysis: JYK, HJH, DCL, THK, JSH; Methodology: JYK, HJH, DCL, JSH, CKP; Project administration: JYK, HJH, DCL, CKP; Visualization: JYK, DCL, CKP; Writing - original draft: JYK, HJH, THK; Writing - review & editing: JYK, HJH.