Assessment of Clinical Symptoms in Lumbar Foraminal Stenosis Using the Japanese Orthopaedic Association Back Pain Evaluation Questionnaire
Article information
Abstract
Objective
It is important to develop an easy means of diagnosing lumbar foraminal stenosis (LFS) in a general practice setting. We investigated the use of the Japanese Orthopaedic Association Back Pain Evaluation Questionnaire (JOABPEQ) to diagnose LFS in symptomatic patients.
Methods
Subjects included 13 cases (mean age, 72 years) with LFS, and 30 cases (mean age, 73 years) with lumbar spinal canal stenosis (LSCS) involving one intervertebral disc. The visual analogue scale score for low back pain and leg pain, the JOABPEQ were evaluated.
Results
Those with LFS had a significantly lower JOA score (p<0.001), while JOABPEQ scores (p<0.05) for lumbar dysfunction and social functioning impairment (p<0.01) were both significantly lower than the scores in LSCS. The following JOABPEQ questionnaire items (LFS vs. LSCS, p-value) for difficulties in: sleeping (53.8% vs. 16.6%, p<0.05), getting up from a chair (53.8% vs. 6.6%, p<0.001), turning over (76.9% vs. 40%, p<0.05), and putting on socks (76.9% vs. 26.6%, p<0.01) such as pain during rest, and signs of intermittent claudication more than 15 minutes (61.5% vs. 26.6%, p<0.05) were all significantly more common with LFS than LSCS.
Conclusion
Results suggest that of the items in the JOABPEQ, if pain during rest or intermittent claudication is noted, LFS should be kept in mind as a cause during subsequent diagnosis and treatment. LFS may be easily diagnosed from LSCS using this established patient-based assessment method.
INTRODUCTION
Lumbar foraminal stenosis (LFS) is a condition seen in degenerative lumbar spinal disorders in which a nerve root or spinal nerve is entrapped in a narrowed lumbar foramen. There is a dorsal root ganglion that functions as a pain receptor at this site making this condition refractory and likely to cause severe lower limb pain10). However, Macnab14) suitably referred to this region as the “hidden zone” and despite major strides in imaging technology today, this site is still often overlooked, making it a factor that can adversely impact surgical success rates.
Nerve decompression sites differ in intra-spinal lesions and foraminal stenosis, and it has been reported that many cases of failed back surgery syndrome are caused by inappropriate treatment of foraminal stenosis4). Conditions that cause L5 radiculopathy include a “double-crush lesion” where the L4/5 level is compressed by an intraspinal canal lesion and the L5/S1 level is compressed by a lateral lesion so that the nerve is compressed at 2 points (medial and lateral), hence the name. However, traditional imaging studies do not allow the clinician to differentially diagnose whether the compressing lesion is inside or outside the spinal canal, or if a double-crush lesion is responsible.
The Japanese Orthopaedic Association Back Pain Evaluation Questionnaire (JOABPEQ)6) provides specific, yet multidimensional outcome measures for patients with low back pain (LBP), including dysfunction and disabilities caused by the disease, as well as resulting psychosocial problems. The reliability and validity of the JOABPEQ have been verified by psychometric evaluations.
It is important to develop an easy means of diagnosing LFS from LSCS. The purpose of this study was to investigate the use of the JOABPEQ to diagnose LFS in symptomatic patients. Our findings from using the JOABPEQ to study clinical symptoms in detail to determine the scale’s usefulness in diagnosing LFS are presented below.
MATERIALS AND METHODS
Thirteen cases (mean age, 72 years) of LFS and 30 cases (mean age, 73 years) of LSCS involving one intervetebral space were enrolled as subjects from among the 143 patients (mean age, 66.8 years) who underwent lumbar surgery between April 2013 and October 2015 at our institution. LFS neuropathy was level L3 in 2 cases, L4 in 2 cases and L5 in 9 cases. LSCS was level L1/2 in 1 case, L2/3 in 2 cases, L3/4 in 5 cases, and L4/5 in 22 cases. LFS was diagnosed by microendoscopic intrapedicular partial pediculotomy in 3 cases15), and posterior lumbar inter-body fusion in 10 cases. LSCS was diagnosed in all patients through lumbar spinous process-splitting laminectomy17). Before surgery, LFS was diagnosed comprehensively based on clinical symptoms, physical findings, plain X-rays, computed tomography (CT), magnetic resonance imaging (MRI), and 3-dementional-MRI (3D-MRI). Foraminal stenosis was defined as: abnormalities such as nerve indentation, swelling, and running transversely in their course through the foramen on 3D-MRI. Ultimately, nerve roots were blocked selectively to diagnose damaged nerve roots based on function. If the visual analog scale (VAS 100-mm method) of the lower limbs was alleviated by 20 mm or less at 30 minutes after nerve root block, the diagnosis was considered positive.
Patient exclusion criteria were as follows: (1) those with residual lower limb pain, (2) those who had previous lumbar spinal surgery, (3) those who had multiple levels of lumbar canal stenosis, (4) those who had myelopathy, and (5) those who had spinal tumor, infectious disease, or spinal trauma.
Clinical symptoms were evaluated using the VAS score for LBP and leg pain ranging from 100mm(extreme amount of pain) to 0 mm (no pain), the Japanese Orthopedic Association (JOA; 0–29 points) scoring system, and the Roland-Morris Disability Questionnaire (RDQ; 0–24 points). The normal JOA score is 29 points, based on 3 subjective symptoms (9 points), 3 clinical signs including straight-leg raising (6 points), and 7 activities of daily living (14 points). The normal RDQ is zero points with the total number of items checked from a minimum of 0 to a maximum of 24.
The JOABPEQ includes 25 questions based on RDQs and Short Form 36 (SF-36).
For Q1-1 through Q4-1 and Q5-1, a score of “1” was considered positive for symptoms, while a “2” or “3” was considered negative. For Q4-2, Q4-3, and Q5-2 through Q5-7, a score of “1” or “2” was considered positive for symptoms, and “3” to “5” were negative (Table 1). Scores are calculated based on the answers to questions in 5 domains: pain-related disorders, lumbar spine dysfunction, gait disturbance, social life dysfunction, and psychological disorders. The score for each domain was calculated according to the official guidelines and ranged from 0 to 100 points, which is deemed proportional to the patient’s clinical condition.
All human and animal studies have been approved by the Chiba University and Shimoshizu National Hospital and have therefore been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. We declare that all patients gave informed consent prior to inclusion in this study.
Statistical analyses were performed with StatView ver. 5.0 (SAS Institute Inc., Cary, NC, USA). For each clinical symptom, differences between both groups were evaluated using an unpaired t-test. For each JOABPEQ item, differences between both groups were evaluated using the chi-squared test. A threshold of p<0.05 was considered statistically significant.
RESULTS
VAS scores (LBP) were LFS: 73±5.17 mm, LSCS: 60±4.67 mm (p=0.105); VAS scores (leg pain) were LFS: 80±5.37 mm, LSCS: 65±5.25 mm(p=0.090); JOA scores were LFS: 15±0.69, LSCS: 19±0.54 (p=0.00047); RDQ scores were LFS: 13±1.30, and LSCS: 11±0.99 (p=0.157). JOA scores were significantly lower (p<0.001) in LFS compared to LSCS (Fig. 1).
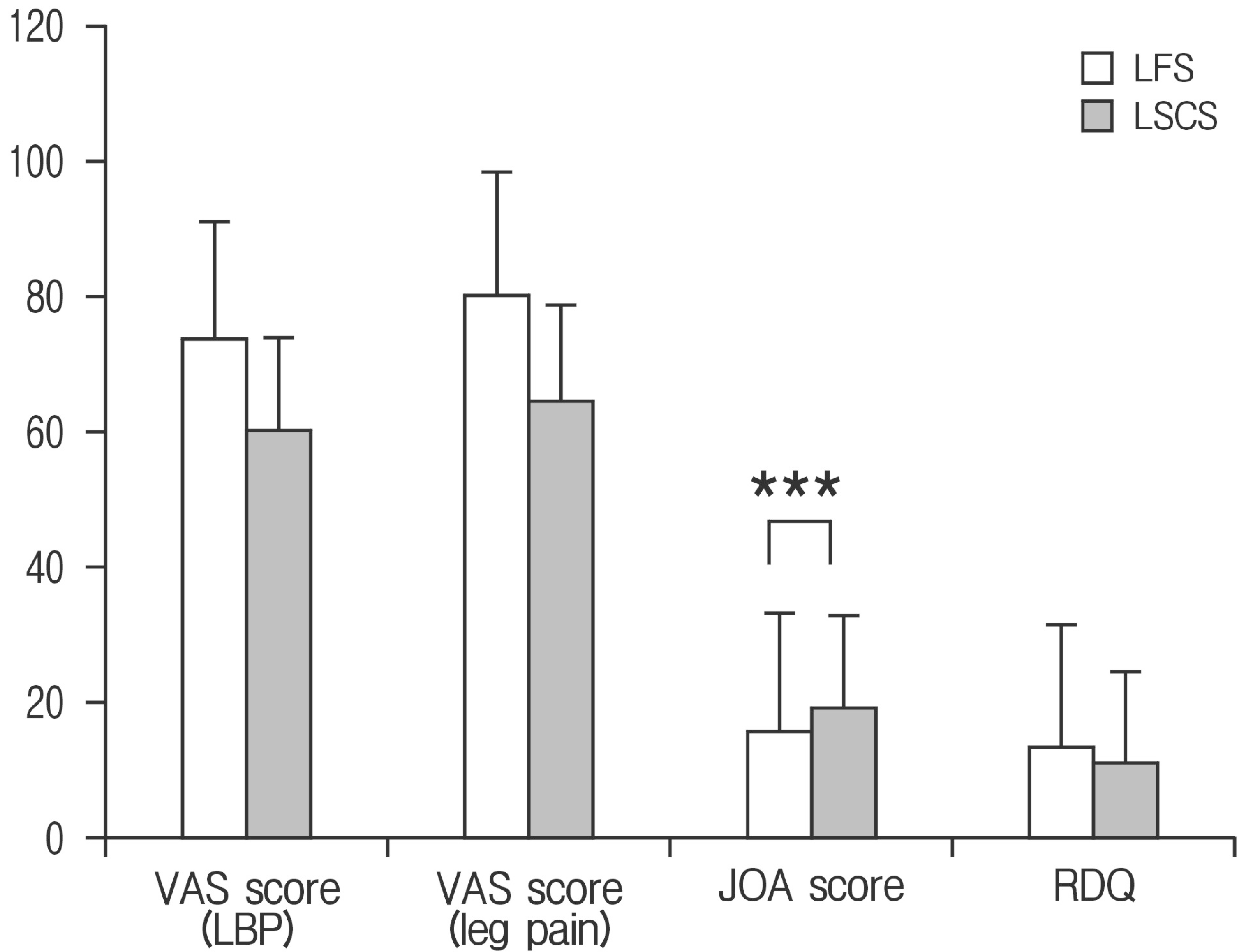
VAS score, JOA score, RDQ in each group. Compared to LSCS, JOA scores were significantly lower (p<0.001) in the LFS patients. VAS, visual analogue scale; JOA, Japanese Orthopaedic Association; RDQ, Roland-Morris Disability Questionnaire; LSCS, lumbar spinal canal stenosis; LFS, lumbar foraminal stenosis. ***p<0.001.
Categories in JOABPEQ include Pain-related disorders LFS: 38±7.48, LSCS: 57±6.51 (p=0.087), Lumbar spine dysfunction LFS: 44±6.86, LSCS: 67±4.22 (p=0.026), Gait disturbance LFS: 28±6.34, LSCS: 41±5.01 (p=0.082), Social life disturbance LFS: 32±5.86, LSCS: 47±3.28 (p=0.009), and Psychological disorders LFS: 35±5.81, LSCS: 43±3.33 (p=0.199). LFS showed significantly lower scores in Lumbar dysfunction (p<0.05), and Social life disturbance (p<0.01) compared to LSCS (Fig. 2).
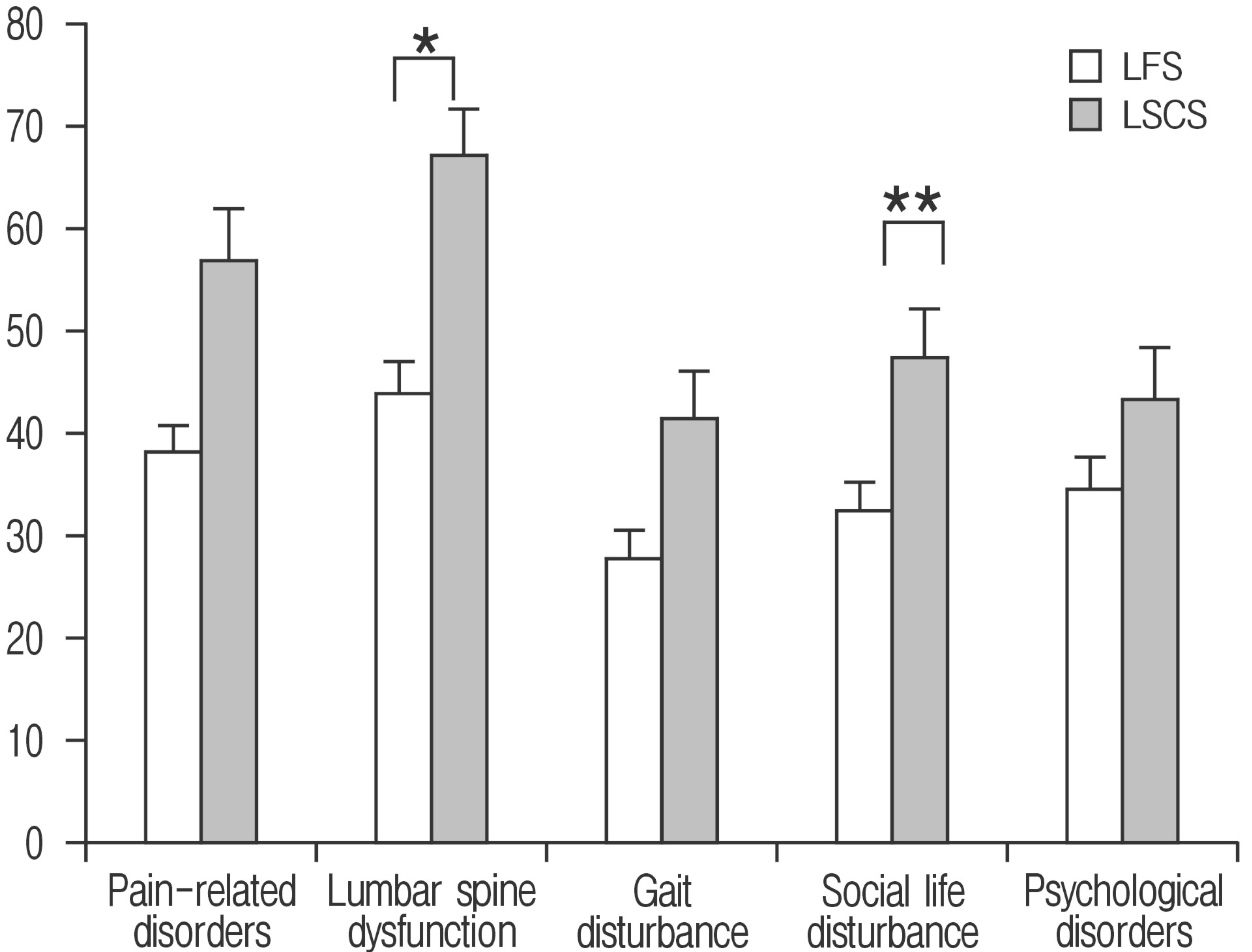
JOABPEQ scores in each group. Compared to LSCS, LFS patients had significantly lower lumbar spine dysfunction (p<0.05) and social life disturbance (p<0.01) scores. JOABPEQ, Japanese Orthopaedic Association Back Pain Evaluation Questionnaire; LSCS, lumbar spinal canal stenosis; LFS, lumbar foraminal stenosis. *p<0.05. **p<0.01.
Statistically significant differences were noted between the 2 groups. Specifically, in Pain-related disorders: (1) have difficulty sleeping: LFS, 53.8%; LSCS, 16.6%(p=0.0125); in Lumbar spine dysfunction: (2) have difficulty standing up from a chair: LFS, 53.8%; LSCS, 6.6%(p=0.0004); (3) have difficulty turning over: LFS, 76.9%; LSCS, 40%(p=0.0261); (4) have difficulty putting on socks or stockings: LFS, 76.9%; LSCS, 26.6% (p=0.0021); in Gait disturbances: (5) have difficulty walking more than 15 minutes: LFS, 61.5%; LSCS, 26.6%(p=0.0298); in Social life disturbance: (6) do not do routine housework: LFS, 38.4%; LSCS, 0% (p=0.0003); and in Psychological disorders: (7) are not in decent health: LFS, 69.2%; LSCS, 30.0%(p=0.0166). There were 7 question items and incidence was consistently higher in LFS than LSCS (Table 2).
DISCUSSION
Appropriately named the “hidden zone” by Macnab14), LFS is often overlooked, accounts for approximately 60% of failed back surgery syndromes, and plays a major role in lowering surgical success rates4). Diagnostic imaging of lumbar spinal canal stenosis involves a comprehensive review of X-rays, CT, and MRI7,12,16), together with functional diagnosis through selective nerve root imaging and infiltration8). Conventional MRI reportedly produces false positives in 30% to 40% of LFS cases and this is therefore a difficult condition to diagnose. Recently, 3D-CT, MR myelography13), 3D-MRI2,20), and diffusion tensor imaging5) have been reported to be diagnostically useful.
Nerve root damage in LFS is most common in the L5 nerve root, accounting for 75% of cases10). There are no useful diagnostic methods to differentiate between possible causes of L5 nerve damage that could be medial stenotic lesions in the L4/5 level, lateral lesions in the L5/S1 level, or double-crush lesions. Electrophysiological tests to measure distal latency of the L5 have been reported. Compared to medial lesions, distal latency is delayed in lateral lesions allowing for a differential diagnosis between the two. However, this is an invasive test and non-invasive diagnostic methods are virtually nonexistent1,9).
Due to DRG involvement in patients with symptomatic LFS, they have generally been recognized as demonstrating more severe symptoms than patients with LSCS3,10,18,19).
In this study we investigated clinical symptoms specific to patients with LFS symptoms. JOA scores were significantly lower in LFS compared to LSCS and lumbar spine dysfunction and social life disturbance in JOABPEQ-measured functionality was also significantly lower in those with LFS.
The RDQ and Oswestry Disability Index are used as specific scales of low-back-pain associated quality of life, while SF-36 and EuroQol are widely used around the world as comprehensive measures of health. JOABPEQ is a patient-based assessment of treatment results that includes both the scientific and psychological aspects4). An excel file can be shared from the JOA website, allowing for automatic assessment of individual patient severity.
Statistically significant differences were noted in 7 of the JOABPEQ domains, namely difficulties in: (1) sleeping, (2) standing up from a chair, (3) turning over, (4) putting on socks, (5) walking for 15 minutes, (6) doing household chores, and (7) remaining in decent health.
In previous reports, Yamada et al.19) found that pain when recumbent, pain on sitting, the Bonnet test, and the Freiberg test were specific symptoms of LFS. Watanabe et al.18) reported that incidences of Kemp test, intermittent claudication, leg pain in a sitting position, and leg pain at night were high among LFS patients. Baba et al.3) reported that all patients suffered from leg pain caused by nerve root involvement, and the incidence of Kemp sign (84.6%), intermittent claudication (84.6%), and leg pain at rest (61.5%) were all high.
Yamada et al.19) developed a support tool to clinically diagnose symptomatic LFS. They assigned an integer score to each identified risk factor as follows: pain when recumbent, 9 points; positive Freiberg test result, 5 points; positive Bonnet test result, 3 points; and pain on sitting, 3 points. For each patient, all applicable risk score values were added for a total risk score which ranged from 0 to 20. Receiver operating characteristic (ROC) curve analysis demonstrated cutoff value was 5 points, and the area under the ROC curve was 0.87435, with a sensitivity of 75.5%, and specificity of 82.3%.
In this study, a high incidence of difficulties were reported in LFS patients such as in sleeping (53.8%), getting up from a chair (53.8%), turning over in bed (76.9%), putting on socks (76.9%) and intermittent claudication such as resting state pain and inability to walk 15 minutes or more (61.5%), findings which do not differ from previously published reports. Our study suggests that if resting state pain and intermittent claudication are noted on the JOABPEQ, an established and widely available patient based outcome scale, further diagnosis and treatment should be considered with potential LFS in mind. By using existing and established assessment methods, it may be possible to diagnose LFS easily in a general practice setting.
We acknowledge that our study has several limitations. First, only a small number of subjects were investigated. Further studies are needed to investigate whether our findings remain valid in a large population. Second, JOABPEQ only assesses lumbar pain and there are no questions related to lower limb pain. Jones et al.11) reported that there was a significant improvement in LBP in patients with LSCS undergoing spinal decompression. In this study, VAS score (leg pain) decreased from LFS: 80±5.37 mm and LSCS: 65±5.25 mm to LFS: 16±5.70 mm (p<0.001) and LSCS: 13±3.11 mm (p<0.001) after decompressed surgery. VAS score (LBP) decreased from LFS: 73±5.17 mm and LSCS: 60±4.67 mm to LFS: 24±7.04 mm (p<0.001) and LSCS: 16±3.30 mm(p<0.001) after decompressed surgery. Not only leg pain but also LBP significantly improved by decompressed surgery in both group (Fig. 3). There are a number of possible explanations for this phenomenon such as improvement of posture, distressed facet joint, and improved nutrient supply to ischemic nerves11). Radicular LBP has been suggested and further investigation into this issue is necessary. Finally, in this study we looked at spinal stenosis in LSF patients, but no comparisons were made with lumbar disc herniation, so further investigations will be necessary.
CONCLUSION
We looked into using the JOABPEQ scale to diagnose LFS in symptomatic patients. Compared to LSCS, those with LFS had significantly lower JOA scores and both the lumbar spine dysfunction and social life disturbance scores on the JOABPEQ scale were also significantly lower. JOABPEQ scores showed a significantly higher incidence of difficulties in: sleeping, getting up from a chair, turning over, and putting on socks together such as resting state pain with a higher incidence of intermittent claudication in those with LFS. Results suggest that of the items in the JOABPEQ, if pain during rest or intermittent claudication is noted, LFS should be kept in mind as a cause during subsequent diagnosis and treatment. JOABPEQ may be used as an easy way to differentially diagnose LFS from LSCS.
Notes
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.