Delayed Spondylodiscitis Presenting as a Skip Lesion
Article information
Abstract
Spondylodiscitis is believed to be caused by an infection that affects vertebral bodies and the intervening intervertebral disc. Usually, typical spondylodiscitis involves a mobile vertebra-disc-vertebra unit, and in most cases, the condition is managed successfully by surgical intervention and intravenous antibiotic therapy. Here, the authors report an unusual case of a spondylodiscitis presenting as a skip lesion, which progressed from L4/L5 to L1/L2, despite open surgical biopsy and empirical intravenous antibiotics. Possible pathogenic mechanisms of this unique case are discussed and a review of the pertinent literature is included.
INTRODUCTION
Spondylodiscitis is an infection of the intervertebral disc space and adjacent vertebral bodies and it can be serious when diagnosis is delayed or treatment is inadequate1). The disease usually presents as a mobile vertebra-discvertebra lesion with or without involvement of adjacent vertebrae2). Our patient had delayed spondylodiscitis that presented as a skip lesion despite continuous intravenous antibiotics. This type of skip lesion is a rare for spinal infections. Awareness of the possibility of a skip lesion should facilitate the prompt diagnosis and adequate treatment of this rare condition.
CASE REPORT
A 64-year-old man with chronic alcoholic liver disease was admitted to Chosun University Hospital with aggravating low back pain and a low-grade fever. On physical examination, he was alert and fully oriented and neurological examination revealed no motor weakness, but severe pain and tenderness in the lower back. Chest radiography findings were normal, and a tuberculin skin test was negative. His body temperature was 37.8°C, and his white blood cell count, erythrocyte sedimentation rate (ESR), and C-reactive protein (CRP) level, were elevated at 10.500 μL, 75 mm/hr (normal, 0–20 mm/hr), and 25.9 mg/dL (normal, 0–10 mg/dL), respectively. Chest X-ray and computed tomography scan did not reveal any parenchymal lung disease or lymph-adenopathy, and sputum acid fast bacilli (AFB) stain showed negative results. Under a presumptive diagnosis of infectious spondylitis, lumbar magnetic resonance imaging (MRI) was performed. MRI of the lumbar spine showed disc destruction at L4–5 levels with severe spondylitis at L4 and L5 (Fig. 1). Emergent open biopsy and irrigation were performed for bacterial culture. Samples were obtained from the intervertebral disc and adjacent vertebral bodies and sent for microbiological and histologic analysis. Microbiological cultures of the specimen, urine and blood cultures, were negative including AFB, but pathological examination revealed chronic inflammation. Hence, vancomycin and ciprofloxacin, which had been previously initiated empirically, were continued after consultation with a microbiologist. A clinical improvement was observed after open biopsy and antibiotic therapy, and he was referred to the infectious internal medicine department for continuous intravenous empirical antibiotic therapy. However, 6 weeks after open surgical biopsy and irrigation, he complained of aggravated back pain and a febrile sensation despite continuous antibiotic therapy. At that time, laboratory data showed a still elevated ESR at 55 mm/hr and CRP at 20 mg/dL. Repeated MRI of the lumbar spine revealed newly developed severe spondylodiscitis at the L1–2 levels and the previous spondylodiscitis at the L4–5 levels (Fig. 2). C-arm guided percutaneous spinal biopsy at the L1–L2 levels was performed using a 11-G bone biopsy needle. However, microbiological results of the culture were also negative. After consultation with the microbiologist, we planned empirical treatment based on continuous intravenous antibiotics. However, he refused further treatment, complaining of aggravated clinical symptoms and radiological findings, and in accordance with his wishes, he was referred to oriental medicine hospital.

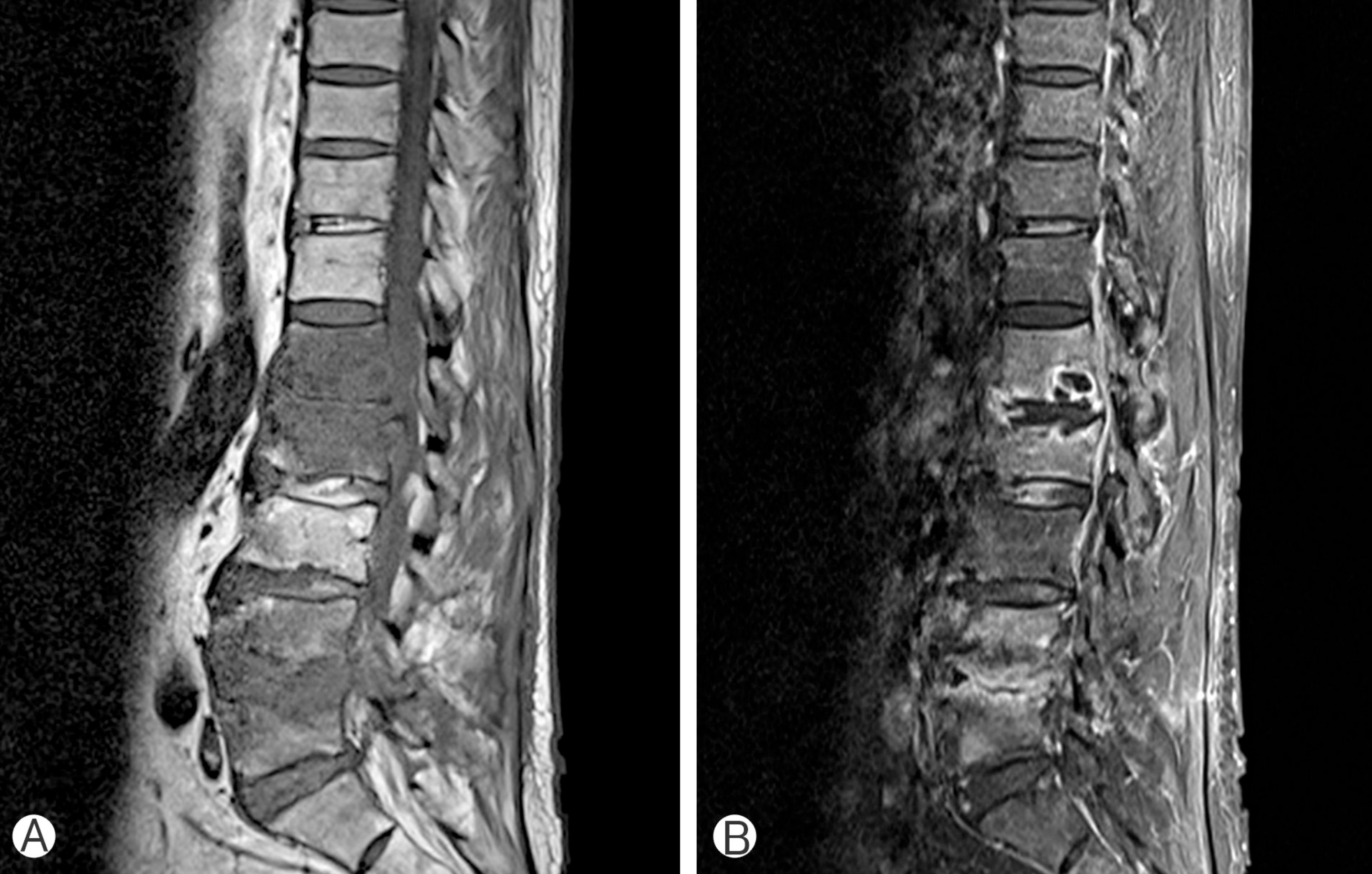
Preoperative T1-weighted (A) and gadolinium enhanced (B) magnetic resonance images show spondylodiscitis at the L4–5 level.
DISCUSSION
Spontaneous spondylodiscitis in adult patients usually present with a history of diabetes, chronic liver disease, or a compromised immune system5). The causative organisms are usually Staphylococcus aureus or β-hemolytic Streptococcus species6,8).
The choice of antibiotics should be based on culture sensitivity testing. However, there is a subset of patients, reported to be 10% to 30% of all cases, who do not grow any organism1). Typical spondylodiscitis is characterized by the involvement of a mobile segment, that is, 2 adjacent vertebrae and the intervening disk with destruction of endplates. Multifocal involvement of mobile segments despite continuous intravenous antibiotics, like that observed in our patient, has seldom been reported. No guideline has been issued regarding optimal antibiotic therapy in patients with microbiologically negative spondylodiscitis, and thus, it is suggested that empirical antibiotics (with staphylococcal cover) should be commenced intravenously. Patients usually require a minimum of 6 to 8 weeks of intravenous antibiotic therapy, and the majority of patients with a pyogenic spinal infection are managed successfully with antibiotic therapy based on culture and sensitivity results. Gillard et al.4) proposed several explanations why discitis patients are sometimes culture negative. They insisted that false-negative biopsy results are influenced by inadequate specimen size. Although it still remains unclear whether open surgical biopsy is superior to percutaneous needle biopsy, open surgical biopsy provides larger specimens for microbiological and histologic studies, and thus, increase the likelihood of detecting an organism. Our patient was a 64-year-old man, whose MRI findings were, extended, skipped level increased signal intensity with contrast enhancement, indicated involvements of L1/L2 and of L4/L5, but microbiological tests, which included open surgical biopsy and histologic tests, were negative. MRI is the single most useful radiologic modality for investigating pyogenic spinal infections, and it is highly sensitive, specific, and accurate (96%, 94%, and 92%, respectively)3). Accordingly, it is currently the investigation tool of choice for the management of spinal infections. Moreover, if the infective parameters remain persistently elevated with intravenous antibiotics, repeat studies including MRI should be considered to find relapse or newly developed spondylitis. Surgical intervention is warranted under a few specific circumstances. These include the development of neurologic signs, spinal instability, vertebral collapse, progressive spinal deformity, an abscess not responding to antibiotics, and failed radiologically guided biopsy necessitating open surgical biopsy7). The goals of surgical intervention are to detect an organism, to preserve neurologic function, and to facilitate stable bony fusion without severe kyphosis.
CONCLUSION
We report a rare case of delayed spondylodiscitis presenting as a skip lesion despite continuous empirical antibiotic therapy. We suggest that a study should be conducted to identify causative organisms and appropriate antibiotic therapies.
Notes
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.