- Search
| Neurospine > Volume 18(4); 2021 > Article |
|
|
Abstract
Objective
To compare the radiological and functional outcomes and complications of adult spinal deformity patients who underwent a pedicle subtraction osteotomy (PSO) below L2 but categorized according to their construct where either 2-rod or multiple-rod construct is applied.
Methods
Sixty-seven patients met the inclusion criteria, and were categorized into 3 groups: 2 rods (2R), multiple rods around the PSO (MRP), multiple rods around the PSO and lumbosacral junction (MRL). Demographic data, operative parameters, spinopelvic parameters, functional outcomes, and complications were collected.
Results
Health-related quality of life scores showed a better outcome at 6 months and last follow-up visits in the MRP and MRL groups which were noted on different domains of Scoliosis Research Society-22 questionnaire, 36-item Short Form Health Surve, and Oswestry Disability Index scores (p<0.05). The 3 groups showed similar rates of rod-related complications with no significant difference (p=0.95). And inside each group, distribution of complications between pseudarthrosis with revision and rod fracture without revision was also similar (p=0.99).
Conclusion
The use of multiple rods across the PSO did not show a better outcome when compared to single rods in terms of incidence and types of mechanical complications. However, better postoperative coronal alignment and health-related quality of life scores in the multiple rods group could be seen demonstrating an improved functional outcome.
Three-column osteotomies such as pedicle subtraction osteotomy (PSO) and vertebral column resection are commonly used for the management of severe spinal deformities. The classical treatment typically used a standard 2-rod construct in order to correct the deformity and stabilize the osteotomy site, however, the important correction potential has been associated to a high instability at the level of the PSO explaining why high rates of pseudarthrosis or implant failure (rod fracture) reaching up to 30% have been previously reported in the literature [1,2]. In addition to spinal osteotomy, other risk factors may be associated with rod fracture such as advanced age, elevated body mass index (BMI), level of the PSO, use of pelvic fixation, more severe sagittal malalignment, and large correction of sagittal parameters [3] in addition to rod extreme contouring that may produce metal fatigue [4]. To palliate such complications, alternatives to the classical Titanium Alloy rod materiel have been proposed such as the use of cobalt chrome [5], but most importantly multiple-rod construct consisting of placing supportive rods across the PSO site to enhance the stiffness and stability have been advocated [6].
The objective of the current study was to compare the radiological and functional outcomes and complications between adult spinal deformity patients who underwent a PSO but categorized according to their construct where either a standard 2-rod or a multiple-rod construct is applied.
This is a retrospective review of a prospective adult spinal deformity database collected from 5 centers. Data from consecutive cases involving patients who underwent thoracic or lumbar PSO with a minimum follow-up of 2 years were obtained, and all patients were enrolled into and Institutional Review Board-approved protocol by the respective sites. Inclusion criteria are: age of at least 18 years, presence of a spinal deformity defined by at least one of the following parameters: Cobb angle Ōēź 20┬░, pelvic tilt (PT) Ōēź 25┬░, sagittal vertical axis (SVA) Ōēź 5 cm, or thoracic kyphosis (TK) Ōēź 60┬░.
Mobility around the PSO site was systematically checked preoperatively (dynamic flexion and extension views, computed tomography scan) in order to ensure fusion in that area postoperatively, therefore patients had either a previously ankylosed spine due to a previous surgery, or in case of mobile levels above or below, anterior support by cages at the aforementioned levels would be systematically done or a modified PSO including the disc above would be performed.
Patients who presented a proximal junctional failure (20 from the initial cohort of 104 patients) were excluded in order to focus on the rods specifically related complications.
Multiple rods technique was defined as using in addition to the classical 2 rods, at least one accessory or satellite rod systematically spanning the PSO area or the PSO and lumbosacral junction (cobalt chrome or titanium).
Demographic data, operative parameters, spinopelvic parameters, functional outcomes, and complications were collected. And complications were distributed into 3 categories: no complications, rod fracture without revision, pseudarthrosis with revision.
Full spine standing anteroposterior and lateral radiographs were made and the different radiological parameters that were assessed preoperatively, at 6 months, and at the last follow-up after the index surgery included: SVA (distance between the C7-plumb line and posterior superior margin of S1), global tilt (GT: angle formed by the intersection of 2 lines, the 1rst line is drawn from the center of C7 to the center of the sacral endplate and the 2nd line is drawn from the center of the femoral heads to the center of the sacral endplate), pelvic incidence (PI), PT, lumbar lordosis (LL), TK, and the coronal C7 plumb line (in relation to the center sacral vertical line [CSVL]). Angles were considered negative if lordotic and positive if kyphotic.
Univariate and multivariate analysis was performed on the relationship between the different rod constructs and the radiological parameters and functional scores using IBM SPSS Statistics ver. 25.0 (IBM Co., Armonk, NY, USA). Student t-test and the Mann-Whitney U-test were used to compare continuous variables. Chi-square and Fisher exact tests were performed for categorical variables. Continuous variables are expressed as mean┬▒standard deviation, and frequency data are expressed as counts and percentages. All p-values were 2-tailed, and p<0.05 was considered statistically significant. Multiple regression analysis was performed to identify risk factors for rods fracture.
For the subjects number, and based on statistical calculations with the use of the following formula:
It was found that when taking into account the initial sample of patients (single rods group) with the known incidence of mechanical complications (around 23%), looking into the number of patients required to see a decrease in the complications rate in the multirods group gave the following results:
- reaching a 3% decrease with a mechanical complications rate of 20% would require 44 patients.
- reaching an 8% decrease with a mechanical complications rate of 15% would require 91 patients.
- reaching a 13% decrease with a mechanical complications rate of 10% would require 231 patients.
Initial data included all PSOs performed in the thoracic and lumbar area (84 patients), however, data analysis showed no complications at all for PSOs above T9 with 85% of single rods being used in this category, in addition, PSOs performed between T10 and L2 included only 2 patients out of 10 with rod fractures with no revision at all. Therefore, and in order to properly compare single rods and multiple rods in a homogeneous sample of patients and avoid any bias, only the PSOs below L2 were included.
A total of 67 patients met the final inclusion criteria and were categorized into 3 groups: 2 rods (2R), multiple rods around the PSO (MRP), multiple rods around the PSO and lumbosacral junction (MRL).
Demographic and surgical data are presented in Table 1. Fifty-three had a prior spinal surgery and mean age at the index surgery was 60 years, with a mean follow-up period of 30 months. The mean number of fused segments was 9. Mean operative time and surgical bleeding were 307 minutes and 1,800 mL, respectively.
The different groups showed a comparable preoperative sagittal malalignment with no significant difference in the different values of GT (p=0.69). From preoperatively to the final follow-up, significant improvements occurred in LL, TK, SVA, PT, GT, and C7-CSVL for coronal alignment (all, p<0.05). Table 2 details the aforementioned radiological data for the whole population. Coronal alignment parameter showed a better value on the last follow-up visit for both MRP and MRL groups when compared to the 2R group with a significant difference (p=0.03) testifying a better long-term coronal alignment. Between 6 months and 2 years, there was no significant difference in the radiological data of the 2 main groups (2R vs. MRP/MRL), however the loss of correction was less in the multiple rods group when compared to the single rod with a LL decreasing from 55.45┬░ to 54.41┬░ and from 53.56 to 50.15┬░ respectively, a GT increasing from 24.57┬░ to 25.84┬░ and from 25.98┬░ to 31.16┬░ respectively and a SVA increasing from 35.71┬░ to 37.13┬░ and from 32.97┬░ to 39.16┬░ respectively.
Health-related quality of life (HRQoL) scores showed a better outcome at 6 months and last follow-up visits in the MRP and MRL groups with globally similar values when compared to the single rods group, and this outcome was noted on different domains of SRS-22, SF-36, and ODI scores (Table 3). This finding was also noted when merging both MRP and MRL groups into a single one and comparing it to the 2R group (Table 4).
Multivariate analysis did not identify specific risk factors for rods complications when comparing the different parameters in the groups. However, a higher tendency for mechanical complications when iliac fixation was performed could be seen.
The 3 groups showed similar rates (between 20% and 23%) of rod-related complications with no significant difference (p=0.95). And inside each group, the distribution of complications between pseudarthrosis with revision and rod fracture without revision was also similar (p=0.99). In fact, around 50% of patients with a rod fracture did not require to be revised (Table 5).
When regrouping the patients and comparing them to the no complication group, higher BMI as a risk factor is identified (p=0.04).
Fixed sagittal or coronal malalignment often requires complex spinal procedures involving the use of 3-column osteotomies such as PSO. PSO technique enables satisfactory correction but at the cost of creating a high iatrogenic instability at the osteotomy site, leading to a high rate of mechanical complications such as pseudarthrosis and rod fractures [7]. Rod fracture is the most frequent mode of hardware failure in long segment spinal fusion surgery, and it can negatively impact the clinical outcome by producing spinal pain, functional compromise, instability, and deformity correction [8].
In order to palliate such disadvantage, the technique evolved over the course of time and the use of multiple rods has been proposed [9]. Initially, a 3-rod configuration was proposed consisting of the classical 2 rods in addition to a central satellite rod independently anchored with laminar hooks to serve as a guide for PSO closure [10]. This was followed by a 4-rod instrumentation based on accessory rod connected by side-by-side domino connectors [3].
The first clinical study that compared a 2-rod construct to a multiple-rod construct showed 17% of rod breakage in the 2-rod group with more than half of the concerned patients requiring revision because of symptomatic pseudarthrosis, whereas only 3% of the multiple-rod group showed partial implant failure without symptomatic pseudarthrosis avoiding the need for any revision in this group [6].
A biomechanical cadaveric study investigated the effect of PSO stabilization with increasing rod numbers and implantation of adjacent cages on range of motion and primary rod strains. It showed that the supplementation of 2 rods with lateral accessory rods [11] coupled to adjacent cages implantation was the most effective strategy in minimizing primary rods strains and even without cages, the strains were significantly reduced [12].
In a study by Shen et al. [13], the dual rods construct consisting of 4 distinct and mechanically independent rods was defended in order to decrease the complications when compared to the use of satellite rods. Their series of 36 adult spinal deformity patients showed 8.3% of rod fractures, and none of them required revision surgery. They advocated the fact that, contrary to the dual construct where all 4 rods are directly on their own pedicle screws, the satellite rods are not, which biomechanically transfers the stress of the reconstruction either proximally or distally resulting in rod fracture above or below the satellite rods.
Another study by Gupta et al. [11] provided a comparison between 2 techniques for rod placement across a PSO and suggested that their described novel 4-rod technique may help to reduce the rates of pseudarthrosis and rod failure.
In a finite element study, the effect of delta-rod configuration on the stiffness and primary rod stress reduction in multiple-rod constructs after PSO was analyzed. Avoiding to bend the third and fourth accessory rods with exact matching of the sagittal shape of the main rod enabled more better biomechanical performance in comparison to other multirods configuration minimizing the loss of fixation after initial rod breakage occurred [14]. Another finite element analysis showed how adding satellite rods increases the rigidity of a construct across the PSO level reducing the stress on the primary rods, with a significant benefit in supplementing medial over lateral satellite rods [15].
The current study eliminated patients who presented a proximal junctional failure from the inclusion criteria in order to focus specifically on the rodsŌĆÖ complications. In fact, proximal junctional kyphosis/proximal junctional failure (PJK/PJF) definitely affects HRQoL, however, it was decided to exclude such complications in order to avoid any bias and specifically study rods related complications and not global complications as PJK/PJF are proximal complications to the construct that may occur with either 2 or multiple rods and are mostly related to sagittal malalignment but are not directly related to the number of rods inside the instrumentation. The current study suggests an acceptable rate of mechanical rod-related complications of 22.4% with a revision rate of 10.4% in the whole population. However, and contrary to the previous papers of the literature, the use of multiple rods across the osteotomy did not prevent pseudarthrosis and fatigue rod fracture when compared to single rods, subsequently showing a similar rate of complications between the 2 techniques.
This finding may probably be related to the fact that the majority of the patients (68%) were operated before with a previously fused spine, and also the systematic supporting of the anterior column, as suggested in the literature, either through interbody cages around the PSO or at the lumbosacral junction, or by performing a modified or extended PSO including the disc above [16,17], which probably decreased rod strains even in the 2R group. The better functional outcome is most probably due to a lesser loss of correction in the multiple rods group; deformity correction seems to be better maintained when multiple rods are used. It has been previously reported that coronal improvement is directly related to better HRQoL outcomes [18].
It should be reminded that with the increased space occupation by the instrumentation, there is proportionally less space available for the placement of bone graft, which may compromise the fusion bed and arthrodesis process.
The addition of extra rods came with a lot of variations in the literature with a significant heterogeneity and lack of convention in describing the constructs as satellite, supportive, delta, outrigger, or accessory rods. This is why a new classification system has been proposed to define the different configurations of multiple rods constructs allowing for standardized communication and research or clinical practice [19]. In our study, surgical technique regarding the use of multiple rods corresponded to the precited definition of using in addition to the classical 2 rods, at least one accessory or satellite rod systematically spanning the PSO area or the PSO and lumbosacral junction which consists of connecting the accessory or satellite rod to the main rod with one proximal connector and one distal connector placed just below the S1 screw in order to protect the adjacent area. An additional detail is to avoid overloading the proximal part of the construct with multiple rods to avoid proximal overload and PJK. In the classification system for multirod constructs [19], satellite rods are defined as additional rods attached to anchors with or without an attachment to the main rod construct, therefore, bridging screws heads that went out of line is considered a satellite rod. Accessory rods are not attached to any anchors but to the main rod via connectors.
In a recent study by Lee et al. [20], 2 groups of adult spinal deformity patients were analyzed according to the occurrence or not of a rod fracture during following-up. They showed that 42% of patients who underwent a PSO presented a rod fracture, while patients characteristics did not have an impact on the occurrence of rod fractures. Use of cobalt chrome rod, accessory rod technique, or lateral lumbar interbody fusion was shown to be effective for reducing the rate of rod fractures. In our study, it was clearly demonstrated that a higher BMI is a risk factor for rod fractures.
A recent study by Dinizo et al. [21] evaluated specifically revision cases that were managed with 2 different posterior techniques. Comparing 2 groups of adult spinal deformity patients, their data demonstrated no difference in fusion grade, or rates of rod fracture and revisions at 2 years, after utilizing a 2 rod versus multiple-rod construct in revision surgery for pseudarthrosis. Such finding goes in pair with our results and clearly demonstrates that the optimal instrumentation configuration is still not identified. Nevertheless, our study showed that despite a similar rate of complications between the different groups, significantly better postoperative coronal alignment and HRQoL scores were noted in the multiple rods groups. This may suggest a more stable construct in the multiple rods group that is preventing secondary loss of correction in the coronal plane and improving the global function of the patient. Such findings will need further research studies in the future in order to be confirmed.
Some limitations of the current study should be acknowledged such as the limited number of patients, the limited number of complications such as pseudarthrosis which may have limited the possibility of comparing the parameters inside the complications group itself. The different types of multiples rods constructs (accessory, satellite) were not analyzed as different subtypes to identify eventual differences as it would have required a bigger number of patients.
The use of multiple rods across the PSO site did not show a better outcome when compared to single rods in terms of incidence and types of mechanical complications. However, a better postoperative coronal alignment and HRQoL scores in the multiple rods group could be seen demonstrating an improved functional outcome.
Fig.┬Ā1.
(A, B) Clinical case depicting pseudarthrosis at the level of the pedicle subtraction osteotomy with 2 rods fractures. (C, D) Postoperative x-rays after revision.
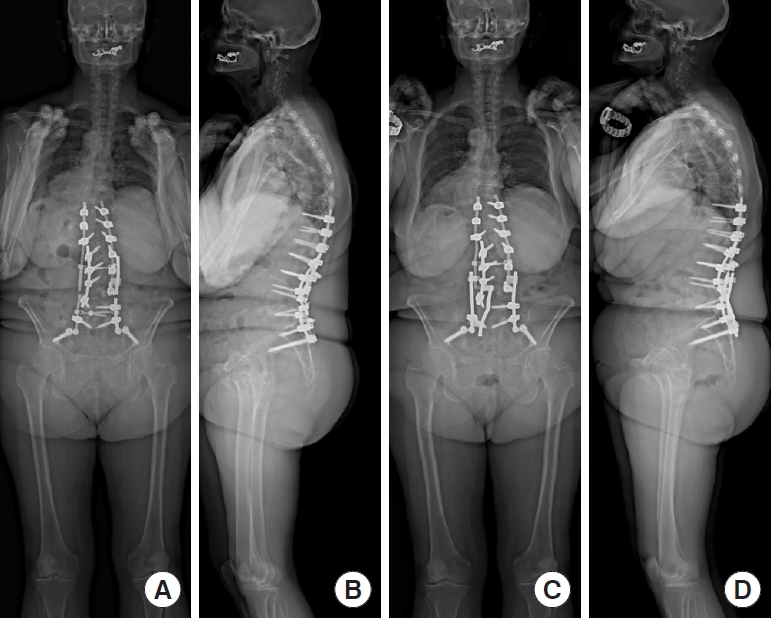
Fig.┬Ā2.
(A, B) Case showing pseudarthrosis at the level of the pedicle subtraction osteotomy and lumbosacral junction with 3 rods fractures. (C, D) Postoperative x-rays after revision.

Table┬Ā1.
Demographic and surgical data of the 3 main groups
Table┬Ā2.
Pre- and postoperative radiological data of total population
Table┬Ā3.
Health-related quality of life scores showing significant difference between the rods groups in favor of the multiple rods (2R, MRP, MRL) at 6 months and 2 years after surgery
Table┬Ā4.
Health-related quality of life scores showing significant difference between the rods groups in favor of the multiple rods (after merging the 2 multiple rods groups together) at 6 months and 2 years after surgery
Table┬Ā5.
Complications of the series (2R, MRP, MRL)
REFERENCES
1. Auerbach JD, Lenke LG, Bridwell KH, et al. Major complications and comparison between 3-column osteotomy techniques in 105 consecutive spinal deformity procedures. Spine (Phila Pa 1976) 2012 37:1198-210.


2. Hyun SJ, Rhim SC. Clinical outcomes and complications after pedicle subtraction osteotomy for fixed sagittal imbalance patients : a long-term follow-up data. J Korean Neurosurg Soc 2010 47:95-101.



3. Smith JS, Shaffrey E, Klineberg E, et al. Prospective multicenter assessment of risk factors for rod fracture following surgery for adult spinal deformity. J Neurosurg Spine 2014 21:994-1003.


4. Tang JA, Leasure JM, Smith JS, et al. Effect of severity of rod contour on posterior rod failure in the setting of lumbar pedicle subtraction osteotomy (PSO): a biomechanical study. Neurosurgery 2013 72:276. -82. discussion 83.

5. Shah KN, Walker G, Koruprolu SC, et al. Biomechanical comparison between titanium and cobalt chromium rods used in a pedicle subtraction osteotomy model. Orthop Rev (Pavia) 2018 10:7541.



6. Hyun SJ, Lenke LG, Kim YC, et al. Comparison of standard 2-rod constructs to multiple-rod constructs for fixation across 3-column spinal osteotomies. Spine (Phila Pa 1976) 2014 39:1899-904.


7. Scheer JK, Tang JA, Deviren V, et al. Biomechanical analysis of revision strategies for rod fracture in pedicle subtraction osteotomy. Neurosurgery 2011 69:164. -72. discussion 72.


8. Palumbo MA, Shah KN, Eberson CP, et al. Outrigger rod technique for supplemental support of posterior spinal arthrodesis. Spine J 2015 15:1409-14.


9. Guevara-Villazon F, Boissiere L, Hayashi K, et al. Multiple-rod constructs in adult spinal deformity surgery for pelvic-fixated long instrumentations: an integral matched cohort analysis. Eur Spine J 2020 29:886-95.


10. Hyun SJ, Lenke LG, Kim YC, et al. Long-term radiographic outcomes of a central hook-rod construct for osteotomy closure: minimum 5-year follow-up. Spine (Phila Pa 1976) 2015 40:E428-32.

11. Gupta S, Eksi MS, Ames CP, et al. A novel 4-rod technique offers potential to reduce rod breakage and pseudarthrosis in pedicle subtraction osteotomies for adult spinal deformity correction. Oper Neurosurg (Hagerstown) 2018 14:449-56.


12. La Barbera L, Brayda-Bruno M, Liebsch C, et al. Biomechanical advantages of supplemental accessory and satellite rods with and without interbody cages implantation for the stabilization of pedicle subtraction osteotomy. Eur Spine J 2018 27:2357-66.


13. Shen FH, Qureshi R, Tyger R, et al. Use of the ŌĆ£dual constructŌĆØ for the management of complex spinal reconstructions. Spine J 2018 18:482-90.


14. Berjano P, Xu M, Damilano M, et al. Supplementary delta-rod configurations provide superior stiffness and reduced rod stress compared to traditional multiple-rod configurations after pedicle subtraction osteotomy: a finite element study. Eur Spine J 2019 28:2198-207.


15. Seyed Vosoughi A, Joukar A, Kiapour A, et al. Optimal satellite rod constructs to mitigate rod failure following pedicle subtraction osteotomy (PSO): a finite element study. Spine J 2019 19:931-41.


16. Bourghli A, Boissiere L, Konbaz F, et al. On the pedicle subtraction osteotomy technique and its modifications during the past two decades: a complementary classification to the SchwabŌĆÖs spinal osteotomy classification. Spine Deform 2021 9:515-28.


17. Schwab F, Blondel B, Chay E, et al. The comprehensive anatomical spinal osteotomy classification. Neurosurgery 2014 74:112. -20. discussion 20.


18. Cawley DT, Takemoto M, Boissiere L, et al. The impact of corrective surgery on health-related quality of life subclasses in adult scoliosis: will degree of correction prognosticate degree of improvement? Eur Spine J 2021 30:2033-9.


19. El Dafrawy MH, Adogwa O, Wegner AM, et al. Comprehensive classification system for multirod constructs across three-column osteotomies: a reliability study. J Neurosurg Spine 2020 Oct 9 1. -7. https://doi.org/10.3171/2020.6.SPINE20678. [Epub].


20. Lee KY, Lee JH, Kang KC, et al. Strategies for prevention of rod fracture in adult spinal deformity: cobalt chrome rod, accessory rod technique, and lateral lumbar interbody fusion. J Neurosurg Spine 2021 Feb 19 1. -10. https://doi.org/10.3171/2020.8.SPINE201037. [Epub].


21. Dinizo M, Passias P, Kebaish K, et al. The approach to pseudarthrosis after adult spinal deformity surgery: is a multiple-rod construct necessary? Global Spine J 2021 Apr 16 21925682211001880. https://doi.org/10.1177/21925682211001880. [Epub].